Endoscopy Equipment
Advances in endoscopy: A journey from diagnostics to therapeutics and AI
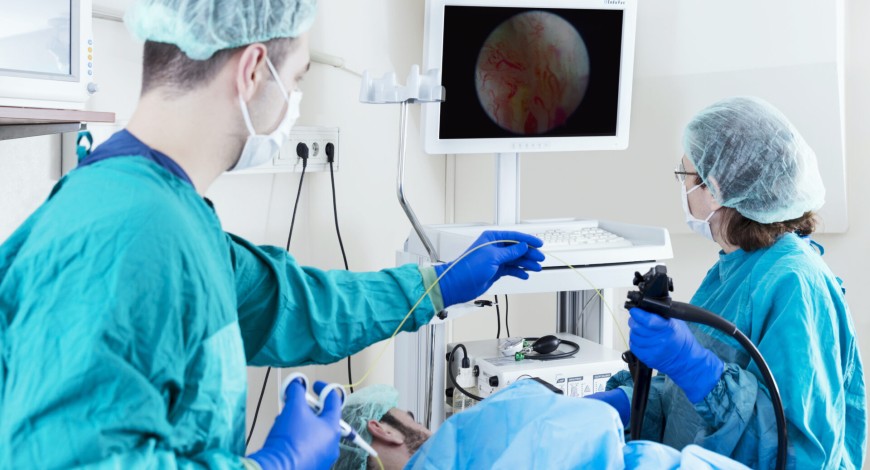
It is humbling to reflect how far the field of endoscopy has come, and thrilling to witness the continued evolution of the field.
Endoscopy has been an integral part of gastroenterology since Basil Hirschowitz created the flexible fiberoptic endoscope in 1956. Endoscopy is currently expanding in a wide range of areas, including diagnostics and, to a greater and greater extent, therapeutics, where it now provides minimally invasive alternatives to conditions that previously required surgical intervention. It can be argued that there is no other subspecialty in medicine, where creativity and imagination are as obvious, encouraged, and limitless as gastrointestinal endoscopy, due to the central location of the gastrointestinal tract within the human body.
Due to the exponential rise of obesity and the metabolic syndrome in Western society over the past few decades, gastroenterology has increasingly delved into the field of obesity-related medicine. As they gain experience treating obese patients medically, bariatric gastroenterologists are now able to offer cutting-edge endoscopic techniques for both treating obesity as a primary condition and treating its complications after bariatric surgery. The American Society of Gastrointestinal Endoscopy’s creation of the Association for Bariatric Endoscopy reflects the growing demand for this procedure. A wide range of endoscopic options are now available, giving patients more choices for managing their weight and the metabolic after-effects of obesity. These options range from simple techniques like intragastric balloons and aspiration therapy to complex suturing and plication procedures.
Finally, the latest frontier in gastroenterology is artificial intelligence (AI). Originally an experimental curiosity, the recent FDA approval of the first colon polyp detection device has brought AI squarely within the reach of everyday gastroenterological practice. Though this only represents the beginning of the wide-ranging impacts of AI in gastrointestinal endoscopy, AI technology can be expected to impact everything from how an endoscopy unit runs to how lesions throughout the GI tract are identified and managed.
It is inspiring to consider how far endoscopy has come, and exhilarating to watch the discipline continue to develop.
Technology trends
Within every industry, the development of new technologies, to greatly expand the end-user’s capabilities and effectiveness, is at the heart of innovation. Seldom does an industry make the requisite technological advancements to revolutionize itself. But when it does occur, everybody from the manufacturer to the consumer exponentially benefits from the quantum increase in practicality, versatility, and usability. The industry that arguably gains the most from such improvements is the medical industry. Innovations within the medical space lead to more noble and tangible benefits as they result in life-changing or even life-saving events.
Specifically, endoscopy is in the midst of a tectonic transition, where continuous innovation has led to instrumentations and methods of the past to be either vastly improved or to grow obsolete. For decades, endoscopic technology has been based on rod lens, fiber, or charge-coupled device (CCD) image sensors. The high price of CCC image sensors, coupled with advancements in complementary metal oxide semiconductor (CMOS) image sensors and wafer level optics technology enabling single-use devices, are two major factors in the changing of the status quo.
As the advancements in medical science expand, so does the frequency and applicability of endoscopic procedures. While once predominantly used within the gastrointestinal field, endoscopic instruments are now used to diagnose and treat issues within the brain, eyes, ear/nose/throat (ENT), spine, heart, urinary tract, and more. These procedures require entry through smaller openings, no bigger than 3 mm, which is impossible to achieve with CCD-based endoscopes.
Some of the recent advances include:
Loop-resisting mechanisms. One of the challenges in modern endoscopy, especially colonoscopy, is the formation of undesired loops in the shaft of a flexible scope. Loop formation impedes expeditious and safe passage to the cecum by transmitting the force of insertion to the colon wall or mesentery rather than to forward progression. Two technical advances aim to prevent loop formation – variable stiffness endoscopes and shape-locking overtubes.
New scope technology. While the construction of standard endoscopes has remained largely unchanged over many decades, novel scope designs are being developed to either simplify colonoscopic examinations or enhance mucosal visualization. Other than double-balloon enteroscopy, these technologies are chiefly limited to small clinical trials, but their application could gain momentum in the coming years.
Self-propelled colonoscopes. In an effort to simplify the process of colonoscopic screening, self-propelled endoscopes are in development. The Aer-O-Scope is a user-independent, self-propelled, self-navigating colonoscope. The device consists of a disposable rectal introducer, supply cable, and a scope embedded within a scanning balloon. A small pilot study examined the proof of concept of the Aer-O-Scope. In a cohort of young volunteers (ages 18–43 years), the device successfully reached the cecum in 83 percent of cases. There were no device-related complications. The device contains no working channel for therapeutic interventions; therefore, it is intended for screening purposes only. Another self-propelled colonoscope, the ColonoSight employs air-assisted propulsion in a disposable system. A pneumatic mechanism generates the pressure to create the forward force while an operator directs the scope using handles. The system uses light-emitting diode optics, rather than video or fiber optics, and has disposable working channels. A pilot study for ColonoSight reported intubation of the cecum in 88 percent of cases at a mean time of 12 minutes, without any device-related complications.
Computer-controlled partially automated colonoscope. The neo-guide endoscopy system is designed to avoid loop formation by adjusting an endoscope’s insertion tube to match the configuration of the colon. The distal tip is guided similarly to conventional colonoscopy, and the insertion tube is comprised of multiple steerable segments connected to an actuation control unit. Using a sophisticated computer program, data from physician-determined tip orientation and insertion depth is used to create a 3-dimensional map of the colon.
Miniature auxiliary imaging device. To detect mucosal lesions, situated behind haustral folds, an auxiliary imaging device has been developed. The third-eye retroscope is passed through the working channel of a standard colonoscope. The 3.4mm device then provides a retroflexed image of haustral folds, a perspective that might be absent when using a forward-viewing colonoscope. In an in vitro study, the auxiliary imaging device was shown to enhance the detection of polyps located on the proximal aspect of haustral folds.
Double-balloon enteroscopy. The double-balloon system consists of a dedicated 200cm endoscope, with a balloon mounted distally and a 145cm overtube with a balloon. The purpose of the overtube is to prevent stretching of the small bowel through which the enteroscope has already traversed. The balloons, whose pressure measures 45 mm Hg when inflated, serve to maintain the position of the scope and overtube. Clinical studies have documented 88 percent success of complete examination of the small bowel in total enteroscopy (upper and lower) cases.
Magnification endoscopy. In magnification endoscopy, a cap with a magnifying lens is fitted to the tip of an endoscope. The mucosa, in contact with the lens, is magnified without impairing the maneuverability of the scope. Degrees of magnification range from 1.5× to 115× and can be changed on the scope by turning a dial at the hand controls. The technique of magnification endoscopy is frequently used in conjunction with chromoendoscopy. Chromoendoscopy is used for broad surveillance of the mucosa, followed by focused examination of suspicious lesions in magnification mode. This combined examination has been reported in case series to enhance detection of Barrett’s esophagus, chronic gastritis, Helicobacter pylori infection, gastric dysplasia, and early gastric cancer.
Chromoendoscopy. The aim of chromoendoscopy is to detect subtle mucosal abnormalities. Commonly used agents include Lugol’s solution, methylene blue, indigo carmine, and Congo red. A 2 percent to 3 percent solution of potassium iodide (Lugol’s solution) reacts with glycogen in keratinized squamous epithelium. Normal squamous epithelium stains a deep brown, but inflammation, dysplasia, and carcinoma do not stain because of a lack of glycogen. Lugol’s solution has been shown to be effective in detecting Barrett’s esophagus as well as screening for squamous cell carcinoma of the esophagus.
Confocal fluorescence microendoscopy. Standard endoscopy uses white light to visualize a large surface area with relatively low resolution. In contrast, confocal endoscopy aims to visualize the mucosa and submucosa with subcellular resolution, a technique deemed optical biopsy. The process of confocal magnification reduces out-of-focus light from above and below the focal plane at a magnification of 1000×. The system is designed to measure tissue fluorescence; therefore, an exogenous fluorophore (a molecule which causes another molecule to be fluorescent) is usually administered. Varying depths of tissue are examined by altering the focal plane, and images from different depths are stacked together to create an optical slice of tissue, thus the term optical biopsy.
Narrow-band imaging. In narrow-band endoscopy filtered light is used to preferentially enhance the mucosal surface, especially the network of superficial capillaries. Narrow-band imaging is often combined with magnification endoscopy. Both adenomas and carcinomas have a rich network of underlying capillaries and enhance on narrow-band imaging, thereby appearing dark brown against a blue green mucosal background.
Autofluorescence. Autofluorescence endoscopy relies on several principles – tissue architecture changes, such as mucosal thickening dampen submucosal autofluorescence; neovascularization alters the light-emitting and scattering properties of surrounding tissue; the biochemical microenvironment, such as high oxidation-reduction activity, alters autofluorescence; and different tissue types have unique distribution of fluorophores. Autofluorescence endoscopy has been shown in pilot studies to improve the detection of dysplasia in Barrett’s esophagus and chronic ulcerative colitis.
Optical coherence tomography. Endoscopic optical coherence tomography is an emerging technology, analogous to endoscopic ultrasound. The technique uses reflection of near-infrared light to produce real-time two-dimensional cross-sectional images of the gastrointestinal tract. These true anatomic images correspond to the histologic layers (mucosa, submucosa, muscularis propria). The images obtained have a resolution 10-fold greater than endoscopic ultrasound. Endoscopic optical coherence tomography is not yet in widespread use.
Light-scattering spectroscopy. Light-scattering spectroscopy mathematically analyzes the intensity and wavelength of reflected light to estimate the size and degree of crowding of surface epithelial nuclei. The technique relies on absorption and scattering of white light. Small clinical trials, using light scattering spectroscopy, have shown efficacy in detecting Barrett’s esophagus and early colonic dysplasia. The technique relies on graphing mathematical computations rather than an optical biopsy in other emerging imaging techniques. Light-scattering spectroscopy might be used in combination with optical biopsy for detection of early dysplasia.
Outlook
A multifunctional endoscope with a variety of imaging technologies will probably become available in the near future. The scope may be switched to autofluorescence mode for guidance to a neoplastic lesion after standard white light has been used for screening and surveillance. Then, with the same scope, an optical biopsy could be performed using confocal microscopy, and the depth of the lesion could be graded using optical coherence. The same scope may have multiple operational channels for interventions, if necessary.
As endoscope applications shift from intralumenal to translumenal therapy, new endoscopic technology captures the imagination. The translumenal operative field could be stabilized, using shape locking tools or guided endoscopes. Other cutting-edge imaging technology could be applied to solid organs for the purpose of detecting neoplastic lesions, and high-resolution and magnifying scopes could improve the optics of an operating field. There will probably be developed scopes, made specifically for translumenal endoscopic surgery. Therefore, as technology advances, so will the applications of cutting-edge endoscopic therapy.











