MedTech
COVID-19 accelerates patient monitoring device market growth
The healthcare industry is shifting its focus to value-based, patient-centric monitoring solutions, providing a fillip to the research of non-contact monitoring technologies.
As the healthcare ecosystem has evolved over the years, one of the major feats has been the acceptance and evolution of patient monitoring systems to augment patient care and improve clinical performance. Assessing the condition or other medical parameters of a patient is essential in making informed clinical decisions. Patient monitoring inside and outside the hospital plays an important role in this process, as the infrastructure connects different modules of the healthcare ecosystem for effective patient care.
Patient monitoring systems have always occupied a very significant position in the arena of medical devices. The increasing medical needs and growing demand for medical facilities are likely to drive patient monitoring systems future market growth.
Advanced technologies in patient monitoring are emerging in response to the increased healthcare needs of an aging population, new wireless technologies, better video and monitoring technologies, decreasing healthcare resources, an emphasis on reducing hospital days, and proven cost-effectiveness. New wireless and Bluetooth technologies, improved infrastructure, and patient familiarity with wireless devices are all combining to advance sales and use of new technologies in patient monitoring systems.
There are a large number of companies offering wireless and remote technologies, patient data processing applications and equipment, or EMR data transfer equipment. Players supplying patient monitoring systems to hospitals are large, established healthcare companies, often working in conjunction with information technology (IT) companies on an entire system.
Healthcare providers are continuing to seek innovative products that can provide greater level of patient care to growing patient population. The move from wired to wireless technology facilitates paramedics, clinicians and medical personnel with a hands-free, wireless device to monitor a patient’s vital signs, creating a safer environment for both EMS personnel and patients. The technology also allows real-time connectivity between the emergency room and medical technician in the field.
Patient data can be transferred through a remote system from the ambulance to the hospital to enable better situational knowledge prior to a patient’s arrival. Wi-Fi based monitoring allows hospitals to leverage existing IEEE 802.11 (Wi-Fi) wireless network infrastructure and investment. A major driving factor is the FDA 510K approval for recently introduced wireless monitoring devices. Low-acuity wearable patient monitoring devices with wireless capability are gaining recognition. They are compact, rechargeable, and provide secure wireless connectivity.
Similarly, implantable cardiac monitors that are used for long term monitoring of a patient’s heart electrical activity have secured FDA approval. These implantable monitors can be connected to smartphone via Bluetooth. The technology provides a new way to monitor for atypical heart rhythms, while staying connected to the doctor remotely.
Indian market dynamics
COVID-19 provided a major impetus to the patient monitoring market, albeit in March and April the ventilators had taken precedence. As the mad rush for ventilators cooled down, tenders were invited end-May onwards for patient monitors. The private sector was absolutely quiet, since they were mostly in a lockdown mode. August onwards the private hospitals, especially ones setting up COVID wards or dedicated areas became active, and as COVID moved to smaller towns, there was demand from those areas too. While the orders from HLL and AIIMS-Delhi, Rishikesh, Bhopal amongst others had been for high-end monitors, the private sector went in for entry level models. This trend is expected to continue, at least till end-2020.
Leading players as Philips trebled their production in both their plants, Germany and China. Some premium brands as GE do not have an entry level model, hence could not take advantage of this windfall. Others as Skanray, BPL, Schiller, and some Chinese brands had a field day. As expected, it was all about meeting demand, price was no longer the only criteria, even for bids invited by the government bodies.
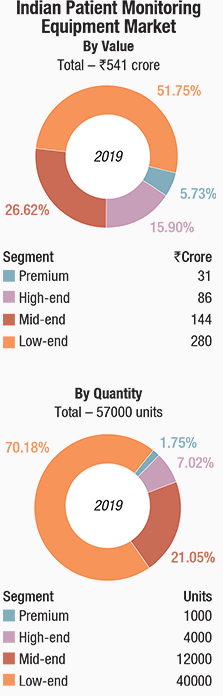 The Indian market for patient monitoring equipment in 2019 is estimated at Rs 541 crore, and 57000 units. The premium segment, of which the super-premium is about 100 units, has an 8 percent contribution by value and a 1.9 percent contribution by volume. High-end systems constitute 15.9 percent share in value terms and 7 percent in volume terms. The belly of the segment continues to be competitively priced systems, the mid-end and low-end segment, and the buying in 2019 seemed to have shifted even more in their favor than it was in 2018. The two segments dominated with a combined share of 91 percent by volume, and 78 percent by value. And a pattern is emerging where 60 percent of the market share is together held by six players, Philips, Mindray, Nihon Kohden, GE, BPL, and Schiller.
The Indian market for patient monitoring equipment in 2019 is estimated at Rs 541 crore, and 57000 units. The premium segment, of which the super-premium is about 100 units, has an 8 percent contribution by value and a 1.9 percent contribution by volume. High-end systems constitute 15.9 percent share in value terms and 7 percent in volume terms. The belly of the segment continues to be competitively priced systems, the mid-end and low-end segment, and the buying in 2019 seemed to have shifted even more in their favor than it was in 2018. The two segments dominated with a combined share of 91 percent by volume, and 78 percent by value. And a pattern is emerging where 60 percent of the market share is together held by six players, Philips, Mindray, Nihon Kohden, GE, BPL, and Schiller.
Global market
The global patient monitoring devices market is estimated at USD 25.76 billion in 2019, and projected to reach USD 44.86 billion by 2027, at a CAGR of 4.4 percent from 2020 to 2027 by Allied Market Research. From past few years, the digital technologies powering patient monitoring devices have widely influenced the operational costs.
The abilities of remote patient monitoring devices to effectively record vital health para-meters will influence the patient monitoring devices market expansion. According to Information Handling Services, by 2020, around 4 million patients monitor their health conditions remotely. This is a 34 percent increase in remote patient monitoring (RPM). Moreover, technological giants such as Google, Apple, and Amazon are tapping into the RPM market; which leads to drastic changes in healthcare. Several remote patient monitoring devices like Mitra, DexCom, and Riverfield are specifically designed for sample collection at home making it easier and cost-effective.
Though most of the markets are dropping down, COVID-19 outbreak has positively affected various healthcare related markets, one of them being patient monitoring devices. At present, the patient monitoring devices market is witnessing tremendous growth. As these devices are playing a crucial role in combating pandemic and monitoring patients. Patient monitoring devices including cardiac monitors, respiratory devices, and temperature monitoring devices are facing a huge demand.
The major key drivers include increase in geriatric population and rise in adoption of remote patient monitoring devices. In addition, surge in prevalence of patients suffering from different lifestyle diseases like diabetes, cancer, and atherosclerosis also contribute toward uplifting growth of the patient monitoring devices market. Furthermore, collaborations between companies, hospitals, and academic institutions are expected to lead to the launch of new products, which would help to increase the market revenue and boost the market growth. However, cost associated with this technology and lack of awareness among patients hinders the market growth. Moreover, government regulations and reimbursement issues can also hamper growth of the patient monitoring devices market.
The cardiac monitoring segment dominated the patient monitoring devices market, governing around 26.08 percent of the global market value in 2019 and its dominance in the market is expected to continue over the 7 years. It is estimated to garner USD 10.25 billion by 2027, registering a CAGR of 4.8 percent from 2020 to 2027. This is attributed to rise in prevalence of various cardiovascular diseases such as congestive heart failure and stroke each year across the globe.
Industry Speak
Advanced hemodynamic management
Anil K Srivastava
Director-Sales & Marketing, Medical Equipment,
Nihon Kohden India Private Limited
COVID-19 has brought some of the most challenging times to all in healthcare settings, in a very short space of time. Clinicians and healthcare staff all over the world have had to adapt their practice in order to manage difficulties such as bed capacity, equipment shortage and staffing issues; not to mention the multifactorial aspects of this novel virus. All at the same time as striving to maintain the same high standards of care to their patients
As coronavirus disease 2019 (COVID-19) spreads across the world, the intensive care unit (ICU) community prepare for the challenges associated with this pandemic. Streamlining of workflows for rapid diagnosis and isolation, clinical management, and infection prevention will matter not only to patients with COVID-19, but also to healthcare workers and other patients who are at risk from nosocomial transmission. Management of acute respiratory failure and hemodynamic is the key.
Hemodynamic monitoring combined with oxygen transport assessment has been used to differentiate the relative magnitude of pulmonary and cardiovascular dysfunction that contribute to hypoxemia, which is of critical importance because therapy directed to correct pulmonary dysfunction (raising the airway pressure) may have adverse effects on venous return and cardiac output.
All patients admitted to the ICU require standard basic hemodynamic monitoring (ECG, heart rate, blood pressure, central venous pressure, temperature, peripheral venous oxygen saturation, blood gas analysis). All critically ill patients need monitoring of intravascular volume status, and intake and output must regularly be observed.
Hemodynamic monitoring is widely used to monitor patient it is segmented into invasive, minimally invasive and non-invasive. Non-invasive Hemodynamic monitoring is growing rapidly now because of very minimal or no risk of infection.
Invasive versus non-invasive hemodynamic monitoring
New non-invasive CCO technology can be used either with IBP or NIBP, enabling continuous, accurate and patient-specific hemodynamic trend monitoring along the entire clinical pathway. Managing and monitoring hemodynamic trends can help improve the quality of care in perioperative, emergency, high-dependency and intensive care settings.
Simplified procedures to improve workflows
New non-invasive Hemodynamic monitoring can also be continuously used and calibrated when patients are undergoing higher-risk procedures and the hemodynamic monitor of choice is more invasive (e.g. bolus thermodilution). Moreover, when the risks surrounding these patients decrease, hemodynamic monitoring can be continue with new non-invasive CCO. New non-invasive hemodynamic monitoring available now in patient monitors, without requiring extra procedures, equipment or additional knowledge for implementation.
Patient monitor trends
N. Manogaran
Vice President–Sales,
BPL Medical Technologies Pvt. Ltd.
Patient monitors with advanced parameters and connectivity solutions are gaining importance in recent times due to global pandemic’s (COVID-19) spread across the world and need for distant monitoring.
We from BPL Medical technologies strive to make the world a better place to live, hence working on the connectivity solutions like technical specs. In addition to that in Last few years we have seen significant increase in demand for additional parameters like IBP and ETCO2. Cardiac output (CO), BIS, NMT, and gas monitoring (AGM) are few other important parameter options that are available with patient monitors.
Cardiac output comes with two technologies one with invasive and the other non-invasive. Invasive technology (thermodilution) is more in demand than non-invasive (ICG). CO has become important parameter for monitoring cardiovascular function.
There are few companies offer 12 channel ECG monitoring/printing for cardiovascular monitoring.
BIS (Bi spectral index) is used to measure depth of anesthesia. BIS uses EEG signals to assess patient’s status of consciousness under anesthesia. Prevent awaking during surgery, drug saving and faster wake-ups as it avoids over-dosage, less PONV (postoperative nausea and vomiting) are the benefits of BIS.
Neuromuscular transmission (NMT) is the transfer of an impulse between a nerve and a muscle in the neuromuscular junction. It is used to locate nerve precisely for giving regional anesthesia. This reduces the time of procedure and provides patient safety and comfort.
AGM (gas monitor) module is used to measure the anesthetic and respiratory gases of the patient under anesthesia. Auto-identification of agent, MAC (minimum alveolar concentration), AWRR (air way respiration rate), Et, and Fi values are the measuring parameters for anesthetic agent. It also provides Et (end tidal) and Fi (fraction inspired) values of respiratory gases CO2, O2, and N2O.
Medical device providers are creating awareness programs to emphasize the importance of the above parameters monitoring for increasing patient safety and comfort. This means more users looking for patient monitors beyond basic 5 or 7 parameters.
Exclusive neonatal monitor is another segment which is rise in demand with focused neonatal care centers and special wards.
Technological advancements and emerging trends
Dr Rajini J
Vice President – Corporate,
Skanray Technologies Pvt. Ltd.
A multi-parameter patient monitoring system is essential for providing intermittent and continuous measurements of patient’s health parameters in places such as emergency room (ERs), coronary care units, intensive care units, and operating rooms.
Patient monitoring has progressed from monitoring when necessary to continuous monitoring of multiple parameters (including vital signs) such as heart rate, electrocardiogram, oxygen saturation level, arterial blood pressure, respiratory rate, body temperature, and capnography, resulting in large amount of unprocessed and unorganized data. The processed data, once made available to clinicians, can help improve the decision-making process and provide efficient, proactive care to the patients. It also reduces human errors, saves time, and helps organisations to focus on sustainable cost optimization.
Shift to patient-centric care for better accessibility and efficiency
Increasing demand for an improved healthcare experience necessitates healthcare efforts be more efficient and reduce the likelihood of additional treatments. Limited follow-up time and reduced hospital stays can control the cost of care for those with chronic diseases such as congestive heart failure, COPD, asthma, and diabetes. Engaging patients with chronic conditions and regular monitoring enables more consistent care, reduce re-admissions, in-patient visits, and fewer emergencies.
Telemedicine
Real-time and remote patient monitoring allows clinicians to remotely diagnose patients, provide a treatment plan, timely communication and quick counseling. It also empowers healthcare professionals to serve remote and less populated areas without having to be physically present in the location.
AI based predictive analysis
Analysis of the sizeable data gathered with monitoring shall be a means of equipping healthcare professional with intelligent assistance for actionable insight. For example, a predictive model using chronic disease patient’s continuous measured parameter can provide a prediction of patient’s disease progression and assist in precision medication. Nowadays with the advancements and adoption of Artificial Intelligence and Machine Learning with real-time data the predictive analysis of the patient condition and patient risk scoring makes patient care better and focused.
Home-based monitoring and COVID-19
There is also an ever-increasing possibility of such monitoring being required outside the hospital setting (e.g. patient’s home). Rise in the chronic disease population and aging population, combined with the COVID-19 outbreak has put a lot of stress on the healthcare system. Given the need to keep low-risk patients out of the hospital in the current pandemic scenario, remote patient monitoring can aid healthcare professionals in monitoring the patient remotely and also ensure individual safety due to reduced exposure. It also helps bring focused care for high-risk patients at hospitals, using the limited available resources. These are the key driving factors for home-based monitoring devices.
In conclusion, real-time and remote patient monitoring reduces stress on the healthcare system, provides better quality of care to patients, ensures personnel safety, increases efficiency, and reduces cost.
The wireless segment accounted for more than 36 percent patient monitoring devices market share in 2019. Wireless monitor near to the patient’s bed can measure and transfer vital sign information to doctors via mobile to immediately check on patient’s health. The wireless monitor eliminates the necessity for separate monitors and is entirely networked with export capability.
As remote patient monitoring devices can be used away for the medical facility to monitor critical parameters of patients, the segment is rapidly gaining popularity among patients with chronic diseases like diabetes, hypertension, and chronic respiratory diseases. Thus, it is expected to be the fastest growing segment, registering a CAGR of 6.3 percent from 2020 to 2027.
The integration of monitoring technologies in smartphones and wireless devices is a key trend in patient care, resulting in the introduction of remote patient monitoring systems, mobile cardiac telemetry devices, mobile personal digital assistant (PDA) systems, ambulatory wireless EEG recorders, and ambulatory event monitors. Advanced devices such as mobile PDA systems enable the real-time transmission of data; for example, real-time cardiac monitoring provides continuous (beat-to-beat) outpatient EKG monitoring for periods ranging up to several weeks.
Remote and wireless patient monitoring devices and technologies can be used for long-term monitoring, such as ambulatory wireless EEG recorders used to detect the epileptiform activity of the patient at home, over a long period of time. These recorders are compact and can store large amounts of data in inbuilt memory cards; they do not restrict the patient’s freedom of movement. Remote patient monitoring devices help enhance patient care delivery and improve patient outcomes for conditions that need continuous monitoring in hospital and non-hospital settings.
Owing to their features and convenience, the demand for wireless monitoring devices is expected to increase across the globe. This, along with the increasing prevalence of heart, neuro, and breathing diseases, has led manufacturers to develop remote cardiovascular, neurological, and respiratory monitoring devices.
The hospitals segment is expected to occupy majority of the market share by end user, and is expected to retain its market position. Owing to the growth in awareness regarding advantages of using remote patient monitoring, the home setting segment is estimated to be the fastest growing segment, registering a CAGR of 5 percent during 2020–2027.
In 2019, North America and Europe were the most lucrative regions of the market, where growth is supplemented by factors such as rise in aging population, increase in prevalence and incidences of patients with lifestyle diseases, and well-established reimbursement policies along with high buying power of customers. The growth pattern in North America is characterized by the stage of market maturity, in terms of both penetration and availability of advanced devices. The Asia-Pacific patient monitoring devices market is estimated to account for the fastest growing sub-segment globally.
The global patient monitoring devices market is highly competitive, and prominent players have adopted various strategies for garnering maximum market share. These include collaboration, product launch, partnership, and acquisition. Major players include Medtronic, Inc., Biotronik, F. Hoffmann-La Roche Ltd., GE Healthcare Ltd, Masimo Corporation, Nihon Kohden Corporation, Johnson and Johnson, Omron Healthcare Co. Ltd., Abbott Laboratories, and Koninklijke Philips N.V.
Opportunity. The healthcare industry in emerging countries will offer significant growth opportunities for manufacturers with the increasing patient population across these countries, coupled with the rising adoption of patient monitoring devices in these countries.
Moreover, emerging countries have registered a sustained increase in the volume of surgical procedures during the past decade, driven by the growing target patient population, the presence of a supportive regulatory environment, and rising medical tourism. Therefore, emerging countries are expected to offer potential growth opportunities to players in the patient monitoring devices market in coming years.
Challenge. There are several risks associated with the use of invasive monitoring systems, such as the discomfort associated with the insertion of monitoring instruments (pulmonary artery catheters). Air embolism, sepsis, bleeding/hematoma formation, cardiac arrhythmias, reduced circulation to the distal limb, hemorrhage, nerve damage (during insertion), thrombosis, air embolism, and pulmonary capillary necrosis are some major risks. These factors increase the mortality rate during invasive procedures.
In addition, the use of invasive monitoring systems is not recommended for elderly and weak patients. Due to the associated risks, invasive monitoring is recommended only for a set of specific indications, provided that the risks associated are overshadowed by benefits of obtaining the relevant data during the procedure. Moreover, invasive monitoring is extremely expensive and requires skilled professionals to perform catheter insertions in patients. Although invasive monitoring provides accurate, comprehensive, and continuous data about the state of patients, the above-mentioned risks limit its usage.
Vendors update
In November 2019, Royal Philips introduced EarlyVue VS30, a vital sign monitor. It calculates risk-based alerts and collects vital signs that will allow identification of subtle signs of patient deterioration to clinicians. The new product launch will strengthen company’s product portfolio and secure its market position, thereby providing competitive edge.
In September 2019, Baxter International Inc. entered into a definitive agreement to acquire Cheetah Medical to improve clinical outcomes with an established patient-monitoring technology to better inform and guide clinicians’ treatment decisions. The partnership will approach to enhance medication delivery and patient monitoring and clinicians will be better able to manage patients with sepsis, acute kidney injury (AKI) and other critical conditions, as well as patients undergoing surgery.
What is the future of RPM?
An increasingly powerful aspect of telemedicine is remote patient monitoring (RPM) – the use of portable, high-tech devices to track and relay data to healthcare providers on such metrics as glucose levels, heart rate, blood pressure, and blood oxygen levels. As this technology continues to evolve, what’s on the horizon? And how will RPM affect the lives of physicians and patients alike?
This technology has the potential to reduce the inconvenience of stringent medication regimens and can be part of creating safer and more standardized processes. This shifts the focus of practitioners and professionals to patient care, since they have more time.
It also helps in improving the efficiency of healthcare and eventually reducing costs. It promises an increase in the accessibility and improves the value of care for both the patients and the care providers.
With this technology, it is easy to reach under-serviced communities. The combination of this technology and other technologies, such as improving the speed of internet connectivity will play a big role in boosting smarter healthcare. Other than providing smarter healthcare, this technology is also going to prove useful in educating health practitioners.
It will be easier for people living in inaccessible areas to access healthcare. This is because the high-tech devices have the ability to break geographic barriers. This greatly improves the diagnosis and management of chronic conditions.
The next trend in RPM technology is miniaturization, a process whereby device makers are making their solutions smaller and less invasive while partnering with new companies expand their market share and grow the technology. As RPM continues to advance, it stands to have a positive effect of the patients on both patients and the health care providers treating them.
Remote patient monitoring will aid in research. For instance, in a study conducted in Italy to evaluate compliance of patients with the required standards, the researchers had a challenge due to lack of accurate data on patients with the chronic diseases from the administrative database. This is because the administrative database does not record the diagnosis for outpatient patients.
As RPM catches on, medical cybersecurity is of paramount importance. Patient information must be protected using the best methods available, steadily updated.
One of the challenges facing this technology is the difficulty of convincing patients to use digital apps. Some patients are not willing to pay for the apps, which can be discouraging for app developers and risk-taking leaders in the field.
Nonetheless, remote patient monitoring has seen great progress since innovation and continues to develop. What challenges there are can be overcome by applying best thinking and best new innovations, like blood microsampling technology, a key element in patient monitoring.
Second Opinion
Patient monitoring systems: How they are is shaping up our time
Dr Niraj Tyagi
Consultant,
SGRH, New Delhi
From being confined to operating room as part of anesthesia monitoring system to wireless remote wearable devices, patient monitoring systems are surely turning futuristic and nimble. Medical decision-making, which traditionally has been considered an intuitive, as well as a scientific, process. Our fraternity now has the opportunity to use AI to in the complex task of medical decision-making. Goal of this should be to provide health care that is personalized and holistic.
One of the goals of bedside patient monitoring is to detect life-threatening events promptly so that they can be treated before they cause irreversible organ damage or death. The longstanding challenge about monitoring has been too frequent alarm alerts leading to alarm fatigue.
The Association for the Advancement of Medical Instrumentation (AAMI), spring 2011 publication reported that 85 to 99 percent of medical device alarms that sound do not require any action at the bedside, yet add to the noise, confusion and stress in an already stressful environment.
New monitoring systems target integration between monitoring parameters, so that alarms are more likely to signal clinically significant conditions, rather than temporary and harmless changes in one parameter. This combined with customization of alarm settings according to patients’ condition and use of AI for pattern recognition is the most likely answer.
The envisaged philosophy of monitoring to measure the degree of injury and to prevent further injury is now also being directed to measure repair. Integration of multipara vital signs with laboratory data and injury or disease specific genomic and proteomic biomarkers can allow monitor the progress of repair. This will help tailor management much early like relooking at antibiotics by integrating inflammatory biomarkers with hemodynamics and bacterial genome identification.
The current pandemic of COVID-19 has taught us many lessons. One of the reasons that lead to higher mortality in Lombardy, Italy, Madrid, and Spain was overwhelming of health care systems despite planned increase in surge capacity. This has brought back focus on concept of resource allocation and value of prognostic tool in earliest phase of disease. Patient monitoring systems and the healthcare systems at large need to recognize this aspect so to be better prepared in case of any such eventuality.
Future trends of patient monitoring devices
J Indhumathi
Superintending Engineer,
Department of Bio Medical Engineering,
Christian Medical College, Vellore
As the healthcare ecosystem has evolved over the years, one of the major feats has been the acceptance and evolution of patient monitoring systems to augment patient care. The increasing medical needs and growing demand for medical facilities are likely to drive patient monitoring systems future market growth along with following technological advancements.
Wireless sensor technology/wearable sensors. Increases the comfort of patients and enabling staff to more easily assist and move them. Federal communication commission announced allocation of a section of the broadcast spectrum for medical body area network (MBAN) in hospitals MBANs transmit a stream of continuous real time data about patient’s condition.
Real time and remote patient monitoring. Telemedicine is becoming a more of reality these days. It enables healthcare professionals to serve remote and less populated areas. With our aging population, the need for monitoring patients, wherever they live and work is increasing, which also reduces expensive hospital stays. There is a growing trend of shifting treatment from hospitals to homes, in order to reduce hospital bills.
Use of big data. Big data is shaking the healthcare industry. It is helping the industry progress in all fronts including precision medicine, predictive analytics, fraud detections and clinical trials. It has affected all healthcare areas from oncology, neurology, genomics, to cardiology. Big data allows healthcare professionals to analyze sizeable medical data sets across a vast population to explore research and treatment opportunities. Big data can help to identify patients who are susceptible to specific conditions and prescribe specific preventive measures to head them off.
IoT. It will allow patients and providers to work together for deeper engagements, open communication and chronic disease management.
RPM sees the potential for growth in a post-COVID world
Physicians have been challenged to reinvent their practices in order to accommodate their patients during the COVID-19 pandemic. The growing market of RPM has become a sought-after solution as indicated by recent increased demand and supply shortages. As such, GlobalData expects the RPM market to double over the next 5 years. As a result of fear and threat of contracting COVID-19, people are avoiding emergency rooms and doctors’ offices for non-COVID-19 health concerns. This is one of the main drivers that is accelerating the growth of the remote patient monitoring market. As such, doctors are not as busy as they were previously and are now partnering with RPM companies to sustain their practices and maintain high-caliber medical consulting.
Businesses are using RPM devices to assess worker health and better gauge their safety to return to work. The Food and Drug Administration (FDA) has issued a new policy expanding healthcare providers’ ability to use non-invasive, FDA-approved RPM devices that measure patients’ body temperature, respiratory rate, heart rate, and blood pressure. Most COVID-19 patients are asymptomatic, so companies are expected to invest in RPM devices to adjust their ready-to-work protocols during the pandemic.
COVID-19 has significantly increased the groundwork for effective RPM usage by physicians and patients. The increased awareness of RPM products due to companies attempting to restart normal business operations is expected to extend to at-home usage by individuals. This acute acceleration of market growth will be sustained by market expansion benefiting payers and providers through economies of scale, increasing ease of use of home-based RPM devices, increasing need for improved healthcare in rural areas, the increasing ageing population and increased incidences of chronic diseases outside of the US and Europe. Future challenges to the growth of the RPM market include educating users and patient non-adherence to medical device instructions.
Outlook
A patient monitor is considered the data powerhouse, capable of accumulating a significant amount of patient data. As the healthcare industry changes to improve competence in providing high quality patient care, there is growing demand for data integration and analytics to improve patient diagnosis and workflow. The future rests in understanding how patient data can fuel new product innovations, and be utilized in artificial intelligence algorithms within healthcare. Rather than making decisions on cloud-based data, emergency protocols could be implemented through decisions made on edge-node data. Moving forward, edge node computing combined with wireless patient monitoring will be considered an advantage for life critical applications.











