Headlines of The Day
How IPHL helped India in strengthening surveillance

Disease surveillance is an essential aspect of public health, enabling early detection and timely response to infectious disease outbreaks. Indian health authorities face the challenging task of effectively monitoring infectious diseases, especially in terms of timely identification and early warning of outbreaks. To tackle this issue, the government introduced the Integrated Disease Surveillance Programme (IDSP) in 2004. The primary objective of the IDSP was to create a comprehensive disease surveillance system that includes both the state and central governments. The programme aimed to identify diseases early and monitor them, which will help inform efficient policy decisions. For instance, during the 2009 H1N1 outbreak, IDSP utilised information and communication technology (ICT) networks for the expeditious collection, analysis, and communication of data. These investments helped to surmount several challenges, including the ability to extend outreach to remote populations, enhance the involvement of the private sector, and augment the use of alternative modes of communication such as e-mail and voicemail.f
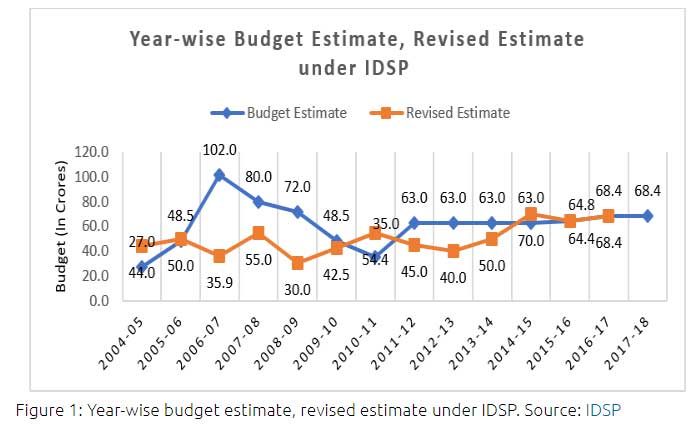
The budget estimate and revised estimate under the IDSP provide an overview of the financial resources allocated to the programme over the years. The budget estimate with a revised estimate, indicates a marginal increase in the budget allocation for the programme (Figure 1). However, the allocation for disease surveillance activities has been inconsistent over the years, with fluctuations observed in the budget estimates.
Subsequently, the Ministry of Health and Family Welfare soft-launched the Integrated Health Information Platform (IHIP) on 26 November 2018. The purpose of this launch was to enhance the IDSP’s digital capabilities. On 5 April 2021, the Union Minister of Health & Family Welfare virtually launched an upgraded version of IHIP. This platform is recognised as the most extensive online disease surveillance system globally, providing real-time case-based information, integrated analytics, and advanced visualisation capability.
To further strengthen surveillance and district laboratories, integrated public health laboratories (IPHL) was established as part of the Operational Guidelines of Pradhan Mantri Ayushman Bharat Health Infrastructure Mission (PM-ABHIM)’ launched by the Hon’ble Prime Minister on 25 October 2021 to strengthen its surveillance and control of infectious diseases. The Government of India provided support to establish IPHL in all the 730 districts of States/UTs in a phased manner under PM-ABHIM. To achieve the objective of ‘Health for All’, IPHL has been established with multi-tiered linkages ranging from local blocks to districts, states, and regional or national level facilities.
IPHLs have the potential to enhance disease surveillance through the provision of guidance concerning the standardisation, integration, and advancement of all-encompassing diagnostic facilities at public health laboratories situated at the district and sub-district levels.
IPHLs have the potential to address the existing health system challenges. To begin with, it should be noted that IPHLs have the potential to enhance disease surveillance through the provision of guidance concerning the standardisation, integration, and advancement of all-encompassing diagnostic facilities at public health laboratories situated at the district and sub-district levels. These can improve early detection and rapid response to disease outbreaks, thereby, preventing the spread of infectious diseases, facilitating clinical management, and widening the scope of surveillance. Secondly, to support clinical decision-making, IPHLs can provide guidance and facilitate the integration of a network of laboratory services at various tiers, including veterinary and public health laboratories. Lastly, IPHLs can provide capacity development and support to peripheral laboratories and block public health laboratories.
While these advancements address existing issues, there is a need to resolve the following inadequacies for their effectiveness. One of these challenges is the social and administrative barriers, i.e., the capacity of current data systems to address significant programmatic and policy inquiries has been restricted. Communication and coordination between laboratories and public health entities can also pose a challenge, particularly during outbreaks when timely and accurate information is crucial. The lack of adequate resources, such as staffing to support laboratory operations remains a challenge. The shortage of trained personnel and limited capacity to handle large volumes of samples can affect laboratory performance.
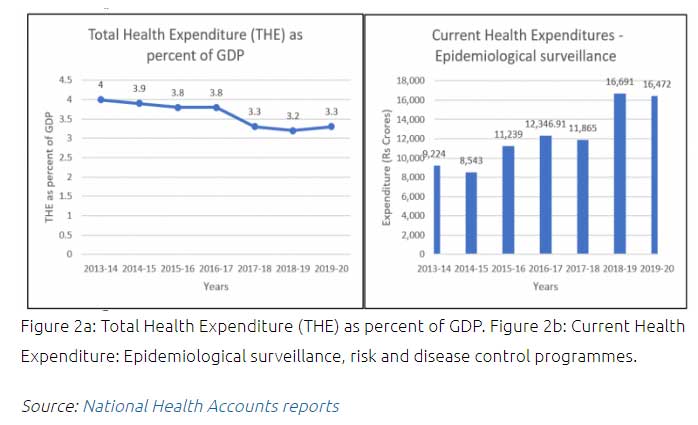
To highlight the underlying factors related to resource constraints, trends of Total Health Expenditure (THE) as a percent of GDP and current health expenditures in epidemiological surveillance are reported below based on National Health Accounts (NHA) data (2013-2020). THE as a percentage of GDP indicates health spending relative to the country’s economic development. Figure 2a shows that there is a relative downtrend in THE as per cent of GDP and Figure 2b illustrates the need for sustained investment in disease surveillance to ensure the efficacy of disease control programmes. Therefore, while advancements have been made in public health surveillance, the lack of adequate resources and inconsistent investment in health and disease surveillance activities remain a significant challenge in India.
Considering the relevance of the context, the authors advocate the PRISM (Performance, Results, Innovation, Strategy, and Management) framework incorporating lessons learnt from across the globe. This enables public health laboratories to focus on improving their performance, achieving measurable results, promoting innovation, developing effective strategies, and implementing strong management practices. Performance indicators enable public health laboratories to track their progress and ensure that their services are meeting the needs of their communities. This can help to improve the quality of laboratory services and ultimately contribute to better health outcomes. For instance, in the United Kingdom, the National Health Service (NHS) has developed a set of key performance indicators (KPIs) for laboratory diagnostic services. These KPIs cover areas such as turnaround times, quality, and cost-effectiveness. By monitoring these KPIs, laboratories can identify areas for improvement and make changes to improve the quality of their services. Aligning laboratory services with broader public health goals and objectives equips public health laboratories to utilise targeted approaches to address the most pressing health issues in their communities. This can help to improve the efficiency and effectiveness of laboratory services and ensure that resources are being used in the most impactful way possible.
Furthermore, by encouraging the adoption of new technologies and approaches, public health laboratories can enhance their efficiency, accuracy, and capacity. This can improve the quality of laboratory services and ensure that public health laboratories are equipped to respond to emerging health threats. For example, Victorian Infectious Diseases Reference Laboratory (VIDRL) has provided a strong commitment to international health programmes through World Health Organization (WHO). In addition, by developing and implementing strategic plans, public health laboratories can ensure that their work is aligned with broader public health goals and objectives. This can help to ensure that resources are allocated effectively and that laboratory services are contributing to the achievement of important health outcomes. In Canada, the National Microbiology Laboratory (NML) developed a strategic plan to outline the laboratory’s priorities and objectives, which include strengthening Canada’s capacity to respond to infectious disease outbreaks and improving the laboratory’s infrastructure and technology. Finally, the PRISM framework emphasises the importance of effective management practices. By promoting strong leadership, workforce development, and quality management systems, public health laboratories can build capacity and ensure that they have the necessary resources to deliver high-quality laboratory services. Given the global benchmarking of best practices, employing the PRISM framework as a means of monitoring the IPHL would be a suitable approach to optimise the health and wellness system.
The adoption of the PRISM framework can also help public health laboratories focus on improving their performance, achieving measurable results, promoting innovation, developing effective strategies, and implementing strong management practices, ultimately contributing to better health outcomes.
Placing surveillance in the context of ongoing discussions, the proposed pandemic treaty highlights the need for improved global surveillance and early warning systems to detect and respond to emerging threats. Therefore, IPHLs can play a critical role in improving disease surveillance, and diagnostic services, and building the capacity of the healthcare workforce. Additionally, the adoption of the PRISM framework can also help public health laboratories focus on improving their performance, achieving measurable results, promoting innovation, developing effective strategies, and implementing strong management practices, ultimately contributing to better health outcomes. Overall, the establishment of IPHLs and the adoption of the PRISM framework offer a comprehensive approach to strengthening India’s public health system and addressing the ongoing challenges of disease detection, surveillance, and control. ORF











