Microbiology Instruments and Reagents
Microbiology, a promising candidate in mNGS
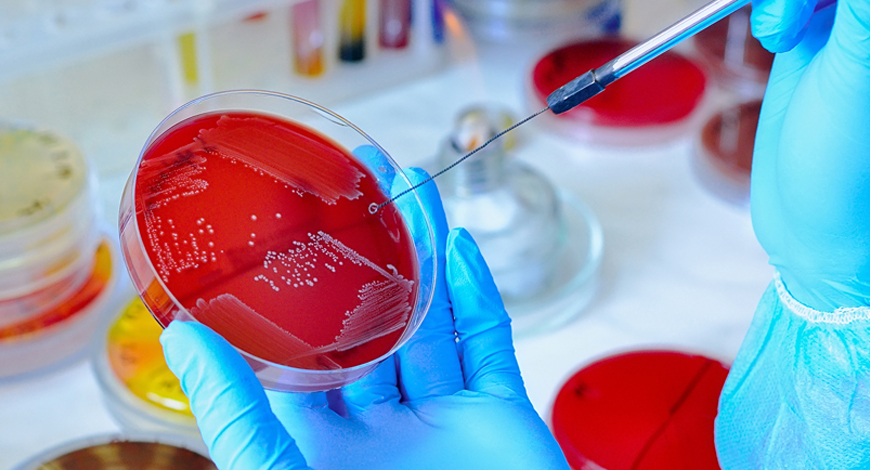
The need for a new diagnostic tool to increase the sensitivity of microbial diagnosis is clear. Although mNGS seems to be a promising candidate, it will take time before it is widely applied.
In the field of clinical microbiology, there have been significant advancements in the use of molecular, genome sequencing-based, and mass spectrometry-driven detection (MALDI–TOF), identification, and characterization techniques. Automation, as well as the integration of information systems for data administration in the labs, is also being implemented. Although there was initially a lot of enthusiasm for these techniques, industry has now moved on to negotiating the obstacles and complications that come with them, rather than just the healthcare benefits. With this in mind, the ongoing process of clinical laboratory consolidation appears to be the right step forward, as it not only covers large geographic areas but also provides an opportunity for the efficient and cost-effective introduction of new lab technologies as well as improvements in translational research and development.
As data increases in bulk and complexity, further technological advancements will change the face of clinical microbiology laboratories. But appropriate implementations in real clinical setup will ensure that the results are faster and cleaner than conventional workflows.
A large, structured repository of bio-banked biological materials from networked libraries will create numerous opportunities for clinical research of infectious diseases and in turn produce impactful healthcare benefits. Consolidation of clinical microbiology laboratories will prove to be advantageous for most aspects of service that distinct institutions already provide individually. Some of the areas that can be aided by innovative and large-scale diagnostic platforms are infectious disease detection, surveillance, and prevention with new translational research and enhanced diagnostic product and service development opportunities.
With testing volumes increasing exponentially, automation is needed more than ever, particularly for small- and mid-sized labs that are in underserved geographic areas. Overall testing volumes are expected to increase 10 to 15 percent per year for the next 20 years, due in part to an aging population that will require more healthcare. The global clinical microbiology market offers significant growth potential for prominent as well as emerging product manufacturers. The global market size is projected to reach USD 4081.4 million by 2028 from USD 3171.1 million in 2021, at a CAGR of 3.6 percent. Technological advancements, rising incidence of infectious diseases and growing outbreak of epidemics, and increased funding and public-private investments, are some of the key factors driving the growth of the clinical microbiology market.
Historically, manual methods were used in culture-based microbiology laboratory testing, and automated methods (such as those that have revolutionized clinical chemistry and hematology in recent decades) were largely absent from the clinical microbiology laboratory.
The adoption of automated methods for culture-based laboratory testing in clinical microbiology has been driven by increased demand for microbiology testing and standardization of sample-collection devices for microbiology culture due to rising pandemic and epidemic outbreaks, as well as a dwindling supply of microbiology technologists. This, in turn, is expected to propel the clinical microbiology market even further.
Emerging markets are expected to offer significant growth opportunities to clinical microbiology product manufacturers and distributors during the forecast period. This can be attributed to the growing prevalence of infectious diseases such as HIV, tuberculosis, influenza, and malaria as well as increasing R&D initiatives to develop innovative genomic techniques for efficient disease diagnosis in developing nations.
The growth in these markets is further supported by improvements in healthcare infrastructure, growing healthcare expenditure, and increasing availability and affordability of low-cost clinical microbiology products. In line with the ongoing trend, several government initiatives have been undertaken across emerging markets to strengthen and expand the healthcare infrastructure.
“Fueled by a limited formulary and reduced ability to timely diagnose resistance, drug-resistant tuberculosis is emerging as a major global health challenge. Furthermore, poorly managed drug-resistant tuberculosis is complicated by poor treatment outcomes and high rates of morbidity and mortality. A rapid diagnosis, together with individualized management, is essential in order scalable treatment options for patients. Whole genome sequencing (WGS) can emerge as the revolutionary one-stop solution for the diagnosis and treatment of tuberculosis in India. WGS of M. tuberculosis isolates allow the detection of drug resistance to all drugs in a single test and also provide insight into the evolution and drug-resistant TB. The WGS technique can determine the entirety of an organism’s DNA in a cost-effective way through a single comprehensive test by enabling an all-in-one approach that provides epidemiological data and comprehensive information on diagnostic background and expected sensitivity of the strains. Dr Mamta Kumari, Chief Microbiologist, SRL Gurgaon.
Diagnostic microbiology tests involve various types of patient samples, such as semen, saliva, tissue, blood, and urine. These diagnostic tests have limited utilization of automated instruments to directly diagnose common pathogens. Clinical laboratories must have proper logistic support for timely sample collection, efficient transportation, and safe and standardized sample processing to provide correct and accurate diagnostic results to patients. However, meeting optimal criteria for sample handling and transportation is a key challenge faced by a majority of clinical laboratories.
The lack of qualified graduates and training programs, particularly in developing countries where demand for skilled professionals is rapidly increasing, may stymie market expansion. However, the introduction of automated systems into the market will eventually replace manually operated traditional platforms, reducing the impact of skills shortage.
The majority of microbiologists would have agreed ten years ago that workflows in a microbiology laboratory could not be automated in the same way that clinical chemistry workflows could. Aside from the differences in sample types and operations, no two microbiology laboratories are same! Today, however, various technologies exist that automate the cycle from incubation through reporting. Microbiologists should value and recognize the opportunity to rethink microbiology and shed some unneeded, longstanding, and established behaviors in a controlled, reflective, and evidence-based manner. It is past time for microbiology to move into the twenty-first century.
Future potential of metagenomics in microbiology laboratories. Rapid and sensitive diagnostic strategies are necessary for patient care and public health. Most of the current conventional microbiological assays detect only a restricted panel of pathogens at a time or require a microbe to be successfully cultured from a sample. Metagenomic next-generation sequencing (mNGS) is increasingly being applied in clinical laboratories for unbiased culture-independent diagnosis. Whether it can be a next routine pathogen identification tool has become a topic of concern.
Since 2008, numerous studies from over 20 countries have revealed the practicality of mNGS in the work-up of undiagnosed infectious diseases. mNGS performs well in identifying rare, novel, difficult-to-detect, and coinfected pathogens directly from clinical samples and presents great potential in resistance prediction by sequencing the antibiotic resistance genes, providing new diagnostic evidence that can be used to guide treatment options and improve antibiotic stewardship. Many physicians recognized mNGS as a last-resort method to address clinical infection problems.
Although several hurdles, such as workflow validation, quality control, method standardization, and data interpretation, remain before mNGS can be implemented routinely in clinical laboratories, they are temporary and can be overcome by rapidly evolving technologies. With more validated workflows, lower cost and turnaround time, and simplified interpretation criteria, mNGS will be widely accepted in clinical practice.
Clinical mNGS has the potential to unbiasedly detect all pathogens in a sample, increasing the sensitivity for detection and enabling the discovery of unknown infectious agents. High expectations have been built around mNGS; however, this technique is far from widely available.
The need for a novel diagnostic tool to increase the sensitivity of microbial diagnostics is clear. mNGS has the potential to revolutionize clinical microbiology. However, its role as a diagnostic tool has yet to be widely established, which is crucial for successfully implementing the technique. A clear definition of diagnostic algorithms that include mNGS is vital to show clinical utility. Similarly, to real-time PCR, mNGS will one day become a vital tool in any testing algorithm.
Research Corner
Scientists identify a new pneumococcal vaccine candidate. Researchers at Karolinska Institutet in Sweden have identified a new vaccine candidate against pneumococci, bacteria that can cause pneumonia, sepsis, and meningitis. The vaccine molecules comprise nano-sized membrane vesicles produced by the bacteria and provide protection in mice, a new study published in PNAS reports.
The pneumococcus (also known as Streptococcus pneumoniae) is the most common cause of ear and sinus infection, and also a major contributor to more severe diseases, such as pneumonia, sepsis (blood poisoning), and meningitis. Pneumococcal infections mainly affect children below the age of two and the elderly, and claim almost two million lives globally every year.
A pneumococcal vaccine has been included in Sweden’s childhood vaccination program since 2009. The vaccine has been developed to protect against severe infections in children, but only targets a fraction of the close to one hundred different types of pneumococcal bacteria that have been described so far.
Since childhood vaccination was introduced, the incidence of severe pneumococcal infections in infants has decreased, an effect that has not been observed in adults.
In this present study, KI researchers examined the possibility of developing a vaccine based on nano-sized membrane vesicles that pneumococcal bacteria naturally produce from their cell membrane in order to communicate with their surroundings and affect other cells. These vesicles contain proteins that help the bacteria to evade the host immune system.
The researchers isolated such vesicles, called membrane particles, from cultivated pneumococcal bacteria. They found that immunization with these membrane vesicles protected mice from getting severe infections with pneumococci.
Moreover, the mice developed protection not only against the pneumococcal strain/type from which the particles were isolated but also against other pneumococcal strains/types.
The researchers identified two proteins in the membrane particles, MalX and PrsA, both of which are essential for the main protective effect.
“Our vaccine candidate – membrane particles containing both these proteins – provide protection regardless of pneumococcal type,” says Professor Henriques-Normark, professor at the Department of Microbiology, Tumor, and Cell Biology, Karolinska Institutet. “The results suggest that membrane particles can be used as a platform for producing vaccines against pneumococcal infections and perhaps other bacterial infections, and this is something we are now working on. There is an urgent need for new vaccine strategies to protect the elderly from pneumococcal infections. The number of severe pneumococcal infections in adults has not decreased significantly, and most of the infections are now caused by pneumococcal bacteria that today’s vaccines do not protect against.”











