Industry
Moving forward with advanced mammography
Advanced techniques in mammography screening, such as AI, tomosynthesis-guided biopsy, contrast-enhanced spectral mammography, as well as a more personalized approach to breast cancer screening, are initiatives that could help reduce the number of false-negatives or positives and drive more accurate early detection of breast cancer.
Breast cancer is the most common cancer in women of all ages, with more than two million diagnoses every year, and a high economic and psychological impact on both the healthcare system and the population. Additionally, male breast cancer should be considered, because even though it represents less than 1 percent of all male malignancies, its incidence has increased by 20–25 percent in the past few decades. Breast imaging is one of the most exciting subspecialties in radiology. The importance of early diagnosis is widely confirmed, and the modalities of breast cancer screening are highly debated, with several guidelines proposed in the world. In these challenging times, a well-established diagnostic–therapeutic care pathway (DTCP) is fundamental to guarantee an essential level of care since the Covid-19 pandemic has caused permanent changes to the practice of medicine.
Currently, the need for personalized medicine has also changed the vision of the field, giving even more importance to multimodality and to the integration of both artificial intelligence (AI) and human resources. Consequently, evaluating the application of radiomics could be of particular interest. Increased mammographic breast density is a well-established risk factor for the development of breast cancer, regardless of age or ethnic background. The current gold standard for categorizing breast density consists of a radiologist estimation, according to the American College of Radiology (ACR) Breast Imaging Reporting and Data System (BI-RADS) criteria. It could be useful to establish the effect of the automated evaluation of breast density with the currently available software. In addition, evaluating how breast cancers are depicted by AI-based computer-assisted diagnosis (AI-CAD) could also be of relevant interest.
Furthermore, examining the real impact of the most recent advancements in standard imaging techniques on breast cancer prevention, such as digital breast tomosynthesis (DBT) and automated breast ultrasound (ABUS), could be incredibly challenging, especially in women with dense breasts. In addition, contrast-enhanced spectral mammography (CESM) could be considered a true alternative to the most expensive MRI. On the other hand, the evaluation of fast MRI could have a great impact on breast cancer prevention, especially in women at high risk.
Indian market dynamics
The Indian mammography market was valued at ₹392 crore in 2021 and is projected to register a CAGR of 10.53 percent from 2022 to 2027, estimates Mordor Intelligence. The major factors contributing to the growth of the market are the rising incidences of breast cancer and rising initiatives by various governments and NGOs to raise awareness about the early diagnosis of microcalcifications in breast tissue. In India, the incidence of breast cancer is increasing, particularly in urban areas among women aged 30 to 40, according to the Indian Council of Medical Research 2020 National Cancer Registry Program Report. Lack of knowledge has caused delays in diagnosis, which has made it a key factor in mortality rates. The Indian healthcare system is experiencing immense progress due to the economic growth, and expansion of ambulatory clinics, public hospitals, and diagnostic centers throughout the country. The penetration rate of diagnostic imaging is increasing with the expansion of these healthcare centers. In urban centers, several Tier-I hospitals are moving from analog mammography techniques to digital tomosynthesis or 3D mammography to decrease the number of false-positives, associated with the analog version. In India, high unmet needs, increasing incomes, rising funding from various public and private organizations, and collaboration between different government organizations are expected to drive the overall growth of the market in coming years.
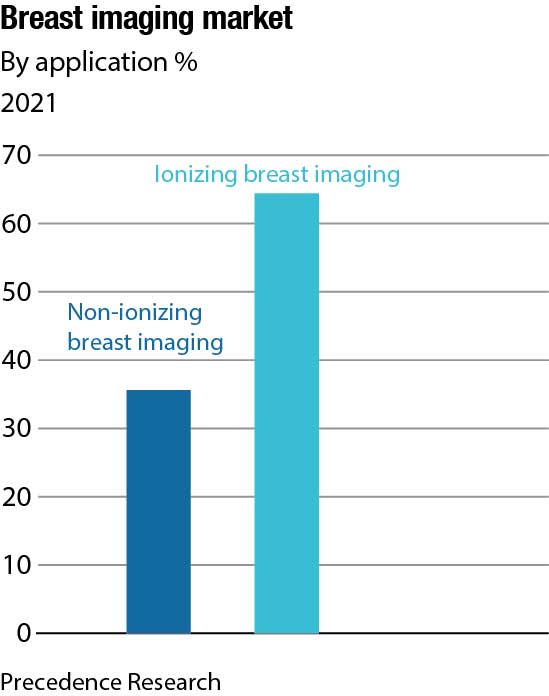
Global market dynamics
The global mammography market size is valued at USD 1.95 billion in 2021, and is expected to grow at a compound annual growth rate (CAGR) of 10.26 percent from 2022 to 2030. The rising prevalence of breast cancer and increasing demand for early-stage diagnosis among patients are some of the key factors anticipated to drive demand for breast cancer diagnostic devices over the next 8 years. Increased access to breast cancer screening systems and growing government initiatives to support clinical interpretation are some of the pivotal factors expected to propel the industry’s growth; such factors are expected to positively influence the industry in the coming years.
| Mammography screening estimates | |
| Regions | Mn nos. |
| Americas | 48.2 |
| North America | 39.8 |
| Latin America | 8.4 |
| EMEA | 19.3 |
| Europe | 17.9 |
| Middle East | 1.3 |
| Russia | 0.0 |
| Africa | – |
| Asia | 34.8 |
| China | 14.2 |
| Rest of Asia | 18.9 |
| Oceania | 1.7 |
| Total | 102.3 |
| Signify Research | October-21 |
The Covid-19 pandemic resulted in significant reductions in cancer screening, cancer management visits, and cancer procedures across the globe. According to a study in the Journal of the American College of Radiology, at the peak of the pandemic in 2020, mammograms dropped to a drastic low, reducing by up to 92 percent. According to the FDA, the number of women examined for breast cancer in 2021 was 38.8 million, implying that hundreds of thousands of women in the US may have missed or delayed screenings owing to the pandemic. This decline in screening volume caused by Covid-19 has presented radiologists with additional challenges.
Digital mammography changing the era of diagnosis
 Satyaki Banerjee
Satyaki Banerjee
Group Chief Operating Officer,
Trivitron Healthcare
A patient can get best treated for any ailment or injury only when the doctor runs out some diagnostic tests/procedures to know the nature of his/her illness or health issue. For instance, healthcare practitioners have mammography as the gold standard screening for early stages of breast cancer in women. Patients can receive it as a diagnostic mammogram, if the same can help the doctor spot any breast concerns or abnormalities in the breast.
Why is digital mammography preferred for diagnosis?
In today’s time, breast cancer in women, having dense breasts, can be detected early without the need for additional tests with the revolutionary type of digital mammography, as it allows the radiologists to get improved fine details of the breasts by minimizing overlapping breast tissues and delivering clinical images of the breast layer by layer.
Digital mammography is an advanced version of film-based mammography for breast-related concerns that have changed the diagnosis era as it provides greater accuracy and peace of mind. It allows the radiologists to capture the images of the inside of the breast and manipulate them so that abnormalities can be easily spotted. The procedure performed is the same as that for conventional mammography. At the end of the procedure of digital mammography, the physician gets to see accurate detailed pictures of any changes in the breast tissues in real time, much before these can be felt by them. This way the physicians can deeply examine the breast condition.
Unlike film-based mammography, the digital mammography system has solid-state electronic detectors that are similar to those of digital cameras and capable of converting X-rays into electrical signals.
Trivitron Felicia full-field digital mammography system is a reliable and superior mammography solution that enables healthcare providers to deliver high-quality patient care with the highest diagnostic confidence. The device is designed using a smart approach to make the procedure less painful for patients, easier for caregivers to handle the procedure, and obtain high-quality clinical images at a very low radiation dose. It provides manual and automatic AEC to select exposure factors to compensate for composition and object thickness.
The repercussions of delayed cancer detection owing to COVID-19 were investigated in a study undertaken in the UK and published in the Lancet Oncology in March 2021. The study covered data from over 100,000 people with breast, colorectal, esophageal, or lung cancer. The study found that 1 and 5-year cancer survival rates will be severely reduced because of the outbreak of Covid-19, owing to the lack of availability of screening services. As a result of lockdowns, screening services were disrupted to some extent, which lowered the demand for mammography systems. This negatively impacted the industry.
As the world’s population is rising, a large proportion of women might reach the age of 60 years or older. Women over the age of 60 years account for about 78 percent of all breast cancer-related fatalities. Breast cancer has a high incidence and fatality rate in this age range, indicating significant unmet demand for breast cancer diagnostics. The need for mammography is likely to rise as the number of events and fatalities rises.
Product insights
The digital systems segment dominated the industry with a revenue share of more than 60.75 percent in 2021, and is expected to witness considerable growth over the next 8 years. Many organizations took decisive measures to manage these diseases because breast cancer patients are at a higher risk of contracting infection. Despite the new technology’s cost being greater than that of conventional systems, digital mammography is becoming the screening method of choice. The 3D systems segment is anticipated to register the fastest CAGR. This is owing to several advantages, due to which hospitals and diagnostic clinics are switching to 3D systems as 2D systems are often ineffective in detecting every sign of cancer, increasing the need for additional screenings, which, in turn, increases the overall diagnostic cost. Moreover, the widespread adoption of 3D systems is owing to technological benefits, such as increased breast cancer detection rates, the ability to manage bigger procedure volumes, and a more advantageous reimbursement scenario.
Furthermore, the trend of 3D mammography system leasing contract agreements is increasing. Rental contract agreements allow end-users to pay a set fee for each 3D mammogram conducted, utilizing 3D mammography technology provided by manufacturers at no cost. This enables low-income hospitals and diagnostic labs to implement this cutting-edge breast imaging technology.
In addition, in recent years, some countries implemented public mammography screening. In these programs, 3D mammography devices are employed to achieve the highest level of accuracy in the identification of breast cancer. Thus, the aforementioned factors are anticipated to contribute to the segment’s growth in the coming years.
The digital mammography segment accounted for the maximum revenue share of more than 66.85 percent in 2021 owing to various advantages of digital mammography technology. Digital mammography is a specialized and sophisticated form of mammography that examines breast tissue for the presence of cancers, using digital sensors and computers rather than X-ray films. In most countries, conventional screen-film mammography (SFM) with a high spatial resolution has been the preferred choice for screening programs. However, with the introduction of digital mammography, a growing number of countries are shifting toward these newer systems, owing to their superior depiction of low-contrast objects, wider dynamic change, and enhanced diagnostic quality of images, particularly when evaluating denser breasts.
Moreover, they also have the added benefit of soft-copy visual displays and soft-copy reading, both of which are easily transferable. Mammography screening is now digital in many nations, including the United Kingdom, providing greater precision, higher quality, and greater efficiency. As a result, digital mammography is becoming the standard screening method, despite the fact that the new equipment is six times more expensive than the traditional systems. Furthermore, in comparison to analog systems, radiation exposure is reduced significantly. The most prevalent type of digital mammography used is full-field digital mammography. It has the potential to make substantial advancements in breast cancer diagnostics, such as lowering radiation doses, reducing breast compression pressure, and improving detection.
The breast tomosynthesis technology segment is expected to witness the fastest CAGR. Digital breast tomosynthesis is a high-resolution limited-angle tomography technology that uses X-rays to create a 3-dimensional image of the breast. It is a new technique that aids in the identification of breast cancer in its early stages. Digital breast tomosynthesis is very useful in analyzing dense breasts, and can enhance the ability to detect breast cancer. It minimizes the number of false-positive readings (readings that identify normal tissue as abnormal) and the necessity for a biopsy.
It is especially good for those with dense breasts. Furthermore, a number of major studies have indicated that combined 2D/3D mammography systems are superior to 2D mammography alone in the diagnosis of breast cancer. A large-scale study of 454,850 patients performed in the US observed that combined 2D/3D combination screening detected 5.5 cancers per 1000 women, compared to 4.3 cancers for 2D screening alone, a 28-percent higher detection rate with combined 2D/3D mammography systems, according to the American Society of Clinical Oncology (ASCO) clinical trial report. Thus, increasing awareness about the usage of these systems, as well as high detection rates, are the primary factors driving the segment’s growth.
North America dominated the global industry in 2021 with a revenue share of around 36.4 percent, and is expected to exhibit a considerable growth rate during 2022–2030. The rising incidence of breast cancer is one of the major factors driving the regional market. However, Asia-Pacific is expected to register the highest CAGR of 9.2 percent from 2021 to 2030.
Recent development
The American College of Radiology (ACR) is set to launch the contrast-enhanced mammography imaging screening trial (CMIST) in collaboration with the Breast Cancer Research Foundation (BCRF) and GE Healthcare. The trial will determine whether contrast-enhanced mammography improves breast cancer detection and reduces false-positive results in women with dense breasts.
About 43 percent of women aged 40 to 72 have dense breasts, which can make detection of breast cancer more challenging, when using mammography alone. The CMIST study seeks to determine if contrast-enhanced mammography (CEM) provides more accurate cancer detection compared to digital breast tomosynthesis (DBT) in women with dense breasts.
CEM combines mammography and vascular-based screening methods in a simple and quick procedure to highlight areas of unusual blood-flow patterns that may indicate malignancy. Early studies of CEM in screening women with dense breasts have shown the potential benefit of CEM in the detection of breast cancer.
As the world observes Breast Cancer Awareness month throughout October, women are encouraged to ‘Don’t Skip’ their annual mammogram – where they can learn more about their own risk factors, including breast density, and consider the best care options with the help of their physician.
AI shows potential in breast cancer screening programs
A major new study in Radiology shows that AI is a promising tool for breast cancer detection in screening mammography programs.
Mammograms acquired through population-based breast cancer screening programs produce a significant workload for radiologists. AI has been proposed as an automated second reader for mammograms that could help reduce this workload. The technology has shown encouraging results for cancer detection, but evidence related to its use in real screening settings is limited.
In the new study – the largest of its kind to date – Norwegian researchers led by Solveig Hofvind, Ph.D., from the Section for Breast Cancer Screening, Cancer Registry of Norway in Oslo, compared the performance of a commercially available AI system with routine independent double reading, as performed in a population-based screening program. The study drew from almost 123,000 examinations performed on more than 47,000 women at four facilities in BreastScreen Norway, the nation’s population-based screening program.
The dataset included 752 cancers detected at screening and 205 interval cancers, or cancers detected between screening rounds. The AI system predicted the risk of cancer on a scale from 1 to 10, with 1 representing the lowest risk and 10 the highest risk. A total of 87.6 percent (653 of 752) of screen-detected and 44.9 percent (92 of 205) of interval cancers had the highest AI score of 10.
The researchers created three thresholds to assess the performance of the AI system as a decision-making tool. Using a threshold that mirrors the average individual radiologist rate of positive interpretation, the proportion of screen-detected cancers, not selected by the AI system, was less than 20 percent. While the AI system performed well, the study’s reliance on retrospective data means that more research is needed.
“In our study, we assumed that all cancer cases selected by the AI system were detected,” Dr Hofvind said. “This might not be true in a real screening setting. However, given that assumption, AI will probably be of great value in interpretation of screening mammograms in the future.”
The results showed favorable histopathologic characteristics associated with a better prognosis for screening-detected cancers with low versus high AI scores. Opposite results were observed for interval cancers. This may indicate that interval cancers with low AI scores are true interval cancers, not visible on the screening mammograms.
The high percentage of true-negative examinations classified with a low AI score has the potential of substantially reducing the interpretive volume, while allowing only a small proportion of cancers to go undetected. By using AI as one of the two readers in a double-reading setting, the radiologist could still identify these cancers.
“Based on our results, we expect AI to be of great value in the interpretation of screening mammograms in the future,” Dr Hofvind said.
Together, these advancements have the potential to be monumental for patients and providers. However, for these technologies to have an impact, the industry also needs to overcome barriers limiting patient access to breast cancer screening. These barriers are plentiful and wide-ranging, including anxiety and fear of pain related to the procedure itself, low income and lack of health insurance, distrust in the healthcare system, limited access to transportation, confusing and inconsistent screening guidelines, and more. Identifying ways to address these challenges will be a priority for the future of mammography, and technology will inevitably play a role in these solutions.
A recent success in this space has been using mammography advancements to improve patient comfort. For some patients, fear of pain and discomfort associated with mammography screening can impact compliance with annual screening protocols. In fact, one survey found 49 percent of women reported fear of anxiety and pain as the reason they never had a mammogram. Therefore, it is expected that innovations in DBT gantries will bring additional features that meaningfully improve comfort, an example of which is the recent introduction of curved breast paddles, which have been clinically proven to deliver a more comfortable mammogram compared to standard compression.
Just as mammography stands as one of the greatest achievements in breast cancer diagnosis and treatment, these advancements are poised to become the next essential tools for radiologists in the fight against breast cancer. Continued innovation is critical to realizing ultimate goal of accurately diagnosing and saving every patient impacted by this disease.












