Daily News
New technologies are transforming ORs
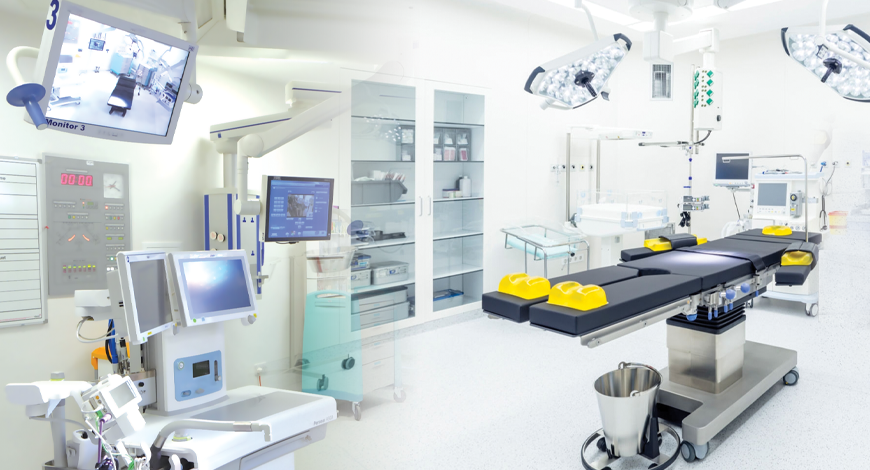
The operating room (OR) is getting smarter, more effective, and a lot less risky for patients. Hospitals are investing in new devices, designs, and digital technologies that promise a new era of innovation for surgery. The moves are part of a growing shift away from traditional open procedures that involve big incisions, lots of blood loss, and long hospitalizations. They point toward a future where more patients can choose minimally invasive outpatient surgeries, with faster recoveries, fewer complications, and less pain and scarring. These new technologies cover a range of advances. With some, surgeons can control robot cameras with eye movements as they move into patients’ bodies through tiny incisions. With others, doctors can create a GPS-like map projected onto a patient’s body to virtually see inside the anatomy before an operation, track their surgical tools and help them operate more precisely.
Other advances aim to reshape the operating room itself, by adding more space for surgeons to work as well as imaging equipment that lets patients receive X-rays and other tests on the operating table, instead of getting shuttled around the hospital. And machine learning and artificial intelligence technology is being developed to let surgeons tap into big data before, during, and after they work, to get guidance from computer systems that have analyzed the procedures and learned to make recommendations.
Of course, many technologies are still in development, and others have yet to be widely adopted or fully evaluated for safety and cost-effectiveness. And some in the healthcare industry warn about embracing new technologies too quickly.
A look into the modern OR
While ORs are one of the most critical areas of a hospital, historically they have had a very low degree of technological savvy. The crucial components of an OR a decade ago were surgical lights, simple operating tables, and critical surgical devices. However, there has been a significant transition, thanks to technology adoption in modern hospitals. An increasing demand for operational efficiency and the need for precision and technology innovation has led to the adoption of automated and sophisticated technologies within operating rooms. Surgical robotics, high-resolution displays, advanced operating tables, and well-integrated network infrastructure now define modern hybrid operating rooms.
Yet despite the tremendous advances made in surgical techniques during the past decade, the equipment and procedures in today’s OR are inefficiently used. Reasons include a lack of compatible and interchangeable equipment and limited communication among surgeons and others on the team, especially during surgical procedures. The operating room is one of the highest-cost centers of a hospital – it can often account for more than 40 percent of an organization’s total expenses. As a result, planners are exploring ways to improve OR efficiency by reducing high, unnecessary costs.
Also changing is the inpatient/outpatient mix of surgical procedures, which has undergone a dramatic transformation in the past 25 years. The average hospital currently performs the majority of its surgical procedures on an outpatient basis; the rising outpatient case mix has significant ramifications for the number, location, and design of operating room suites. However, the days of the hospital may be numbered. In a shift away from their traditional inpatient facilities, healthcare providers are investing in outpatient clinics, same-day surgery centers, free-standing emergency rooms, and micro-hospitals, which offer as few as eight beds for overnight stays. They are setting up programs that monitor people 24/7 in their own homes. And they are turning to digital technology to treat and keep tabs on patients remotely from a high-tech hub. One of the key drivers of outpatient migration – and the most important trend in surgery across the past three decades – has been the shift toward minimally invasive surgical (MIS) techniques. OR design has evolved in concert with MIS, resulting in integrated MIS suites with streamlined equipment and image-visualization technology.
Such next-generation technologies are altering surgical paradigms like the introduction of robotic surgical systems, and they are producing significant market-share swings in many localities. Also, imaging technologies like surgical navigation systems are projected to become more ubiquitous in operating rooms of the future.
Hybrid ORs. Hybrid ORs have been surging in popularity over the last couple of years. Their market globally is expected to surpass USD 1 billion by 2024, growing at an average CAGR of 13 percent. Also referred to as the operating room of the future, a hybrid operating room is considered to be a mix of a minimally invasive room, general surgery room, CAT lab, and endoscopy room. This configuration enables procedures like flexible endoscopy, laparoscopic surgery, and interventional radiology.
A critical push for hybrid operating rooms came after the evolution of radiology techniques in modern medicine. Rather than have radiology as a separate room or department, it was integrated inside the operating room itself. The idea was to monitor the surgery live, similar to anesthesia.
It is crucial to understand the underlying considerations that paved the way for the emergence of a hybrid operating room – enhanced visualization in the surgical theater, thereby decreasing the probability of a diagnostic error. Images transmitted on live screens as those during endoscopy procedures are now much more popular with surgeons. In the past, badly-positioned surgical lights and other equipment resulted in shadows and blurry visuals – notably when doctors conducted procedures using the naked eye alone. This problem has been addressed with the use of HD cameras, putting the surgeon back in control. Surgical headlights are also becoming increasingly popular as they are small, non-intrusive, and help augment the surgeon’s vision – resulting in much better visual detail overall.
Augmented reality. In the neurosurgical operating room, augmented reality (AR) currently comes into clinical effect together with the microscope. Tumors and other enriched objects are injected into the microscope’s ocular so that the surgeon can see what lies under the visible surface. This does not just apply to larger anatomical structures, but also to those that cannot be seen with the naked eye like fiber tracts that are near the treatment area. If the surgeon is using an exoscope, these views are visible to the entire team from its monitor. The beauty of AR is that in seconds, the surgeon can call up additional information about the patient and the case. Augmented reality in the OR has the potential to positively change the way a surgeon consumes and experiences data.
Robots and AI. About a dozen robots built for the OR already assist with hip and knee surgeries and specialized procedures like spinal, abdominal, or laparoscopic surgeries. Intuitive Surgical’s da Vinci robotic system has been in operation for almost two decades and has performed more than six million colorectal, thoracic, and other minimally invasive operations where major surgeries used to be required. While robots in the OR are not new, robots will soon help doctors reach patients who otherwise would not benefit from them, thanks to robust and hyperfast 5G cellular networks that are coming. As just one example, remote surgeons will be able to use robots as their eyes and hands in disaster zones and distant clinics.
And the field is about to explode with new models designed to operate on eyes, hearts, and brains. Some 40 companies are making robots and are expected to be in the market in the next 5 years. More surgeons will be adopting robotic assistance because they are recognizing this is the next generation of tools to help them do their job better.
Also, artificial intelligence will play a significant role in robotic and traditional surgeries. For example, AI systems could analyze thousands of hours of surgical videos to develop custom procedure planning. When combined with augmented reality, computer vision-equipped AI could detect anatomical structures like major nerves, and alert surgeons nearing them to keep their cutting instruments away.
Virtual reality training. These new technologies are also crucial for advancing education. VR visualizations are already helping train surgical teams for new procedures and instruments before they enter the operating room. They can also assist surgeons in planning complex operations and help doctors communicate with patients, who can view a pre-op simulation of the surgery through a VR headset.
Made-to-order instruments. Surgical procedures are not the only parts of the OR going digital. Rapid advances in 3D printing – where layers of metal or polymer materials are deposited on top of each other to create complex designs – could soon change how surgeons get tools in their hands. Today, hospitals must order and stock surgical tools from distant manufacturers in a process that is often wasteful and inefficient, because specialized tools come in kits that can contain instruments the surgeon does not need. But researchers are pushing forward with ideas to 3D print instruments on-demand with no stockpiling, shipping, or unwanted kit components.
Way forward
At first glance, the future prospects for the hospital industry’s surgery business look promising. Profit margins for most procedure lines remain solid, and an aging population will fuel growth in a broad array of surgical interventions. However, demographic trends are not the sole drivers of surgery volumes – technological and competitive forces will also exert a significant influence on the future course of surgery. On the technology front, advances in biomedical engineering will create new surgical interventions while rendering existing surgical procedures obsolete. Technological innovations will also redefine how surgery is performed. Patient demand for less invasive procedures has already spurred the development of new techniques as single-incision laparoscopy and natural orifice-based endoscopic surgery. In addition to minimizing the invasiveness of surgery, surgeons will demand more advanced imaging modalities to improve the precision of their operations.
Competition is likely to intensify in key service lines. In particular, as the inpatient-to-outpatient migration of surgery continues at a gradual pace in the coming years, freestanding surgery providers will target short-stay inpatient procedures in orthopedics, bariatrics, and other lucrative procedural areas. Even as hospitals prepare to defend their profitable inpatient surgery base from new competitors, the looming shortage of surgeons could pose a daunting challenge to sustaining a robust surgery business.
The field of surgery is evolving very fast, and technological advances are making it more efficient and effective and improving patient outcomes. While surgery may never be fully automated, in the future, robots will be smarter and more interactive, bringing as much information to surgeons as possible during surgery. Of course, many technologies are still in development, and others have yet to be widely adopted or fully evaluated for safety and cost effectiveness.











