Cath Labs
Novel technologies head toward accuracy
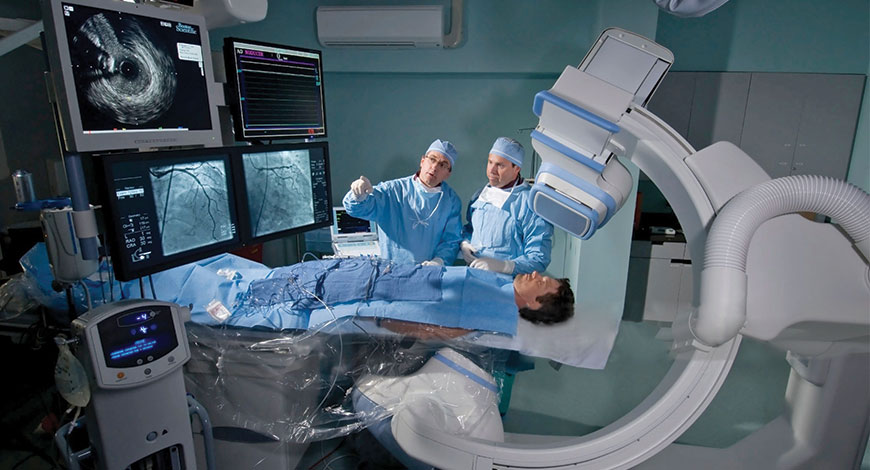
No one can predict for sure, but one thing is certain: the healthcare delivery of the future will require a willingness to think creatively and investigate out-of-the-box solutions.
Recent years have seen a huge array of new procedures performed in the cardiac cath labs and in a variety of similar interventional suites in other areas of the hospital: valve repairs and replacement, closure of a number of congenital heart defects, peripheral vascular interventions for limb and cerebral vascular obstruction, mechanical approaches seeking to prevent arterial embolism from the heart or dissolving thrombi already present in the peripheral and cerebral arterial circulation. Other catheter interventions include a range of approaches for managing venous disease as well as cardiac electrophysiology procedures seeking to control atrial and ventricular arrhythmias. The volume of these procedures is increasing every year, resulting in a lessened need for so-called open operations for many individuals with cardiovascular disease.
Practitioners are no longer cardiologists alone. Indeed, a considerable number of radiologists, vascular surgeons, and cardiothoracic surgeons are now performing interventional procedures in the cath lab and in specially designed interventional suites. The cardiac cath lab has now metastasized and is found in radiology departments and operating rooms. It is expected that this trend will continue in the future, leading to shorter hospitalization, less morbid interventions, and shorter times for patients to recover from procedures.
 Dr Vivek Chaturvedi
Dr Vivek Chaturvedi
Senior Consultant, Cardiology
and Director Cardiac Electrophysiology and Pacing,
Narayana Hospital
“India is the worldwide capital for diabetes and heart disease. It is no surprise, therefore that the need and demand for cardiac services and equipment continues to rise. A cardiac catheterization laboratory is an integral part of any contemporary large cardiology service. With increasing longevity and percutaneous solutions for several cardiac problems (e.g. TAVR), the utilization of cardiac catheterization services in India is expected to rise even further. With rapid advances in diagnostic and interventional techniques and technology, the cardiac cath lab continues to be updated with newer equipment, like OCT, IVL, and laser systems. Also newer cath labs are achieving remarkably low radiation exposure without compromising safety. Hence the cathalb equipment industry, in my opinion, is poised to grow further and have exciting times ahead. Issues that need addressing though remain; expensive after-sale-services as well as the need to standardize safety and training practices for cardiac cath lab personnel”
There have been tremendous advances in 3 dimensional (3D) technologies in the past few years, not only in various medical and surgical fields but also in our daily lives outside of work; with more and more new features in cellphones, computer design programs, and movies. 4 dimensional (4D) imaging captures 3D images over time. These technologies are particularly important in cardiology, especially in interventional cardiology. The heart is a very dynamic organ and understanding the variation in the anatomy of vessels and geometry of cardiac structures is key to ensuring successful procedures, patient’s safety, and good outcomes. More recently, newer innovations in both 3D and 4D technologies have been developed, some of these innovations and how they can be potential game-changers in the cath lab are:
3D holograms. It converts live transesophageal echo (TEE) imaging into real-time 3D holographic video in the cath lab to aid structural heart procedures. The 3D hologram is projected on a special display screen, and the interventional cardiologist uses hand movements and a foot pedal/switch to change the image orientation without breaking the sterile field. It also allows the operator to see the tools they use in the cath lab, including catheters or devices, in real-time in a 3D format. This technology does not even require the user to wear 3D glasses.
HeartFlow planner. This is a noninvasive, real-time virtual tool for coronary artery disease intervention. It allows interventional cardiologists to virtually map vessels on a 3D coronary tree, with color codes indicating the fractional flow reserve-computed tomography (FFR-CT) values for each vessel as measured by a computational fluid dynamics algorithm. This seems to be a good tool for percutaneous coronary intervention (PCI) planning in vessels with significant disease; as it aims to provide us with a non-invasive way to determine whether a stenotic lesion if potentially flow limiting. However, CT-FFR has its own limitations, and some patients might still need invasive FFR for accurate assessment.
 Dr Sameer Gupta
Dr Sameer Gupta
Director, Cardiac Cath Lab,
Metro Group of Hospitals
“There has been an explosion of heart disease and other lifestyle related diseases over the few decades. Cardiovascular diseases remain the primary cause of mortality in adults across the world. In the post COVID world, the government has taken major steps COVID has further improve healthcare delivery across the country. This is not just in metro but also tier II and tier III cities. The PMJAY will also enhance primary, secondary, and tertiary care delivery. The cath lab industry will flourish with increased number of labs being set up to meet the demands in tier II and III cities. With advent of newer procedures like TAVR, mitral clipping, and left atrial appendage occlusion the existing labs will also be upgraded to improve imaging quality while minimizing radiation dosages. Labs integrated with IVUS, OCT, and superimposition of CT and TEE images on the cath lab images will start gaining steam”
3D printing. 3D printing has been used in the surgical fields for more than a decade. It refers to making complex 3D objects from computer-aided designs. This technology has been increasingly utilized in structural heart procedures in the past few years, where these 3D models can be printed from a patient’s CT, MRI, or 3D ultrasound images. These 3D printed structures not only help with procedural planning and device sizing but also allow operators to practice dry runs and perform pre-procedural navigation.
4D imaging. It adds an important component to 3D imaging, which is the change of these 3D images over time. 4D flow images include the direction of blood flow, blood velocities and shear wall stress. This is particularly important in coronary interventions, structural heart procedures, and different congenital abnormalities where identification of blood flow in the 4D view is useful, especially when the anatomy is complex. These changes in position over time help guide our procedures, not only to ensure successful outcomes but also to avoid potential complications. These 4D images require large amounts of data, but they can be obtained from either cardiac MRI or computational fluid dynamics, which is a specialized area of mathematics and fluid mechanics in engineering. 4D imaging is still in its early phases, but it is another exciting advancement in the field.
With continued collaboration with informational technology experts, engineers, and scientists, these innovations are potentially game-changers in different fields, including coronary interventions and structural heart procedures.
The overall trend in the cardiac output monitoring market is a movement toward noninvasive or minimally monitoring methods. Some of the recent trends include:
Advances in cardiac output monitoring devices. Various patient groups need highly accurate estimation of cardiac output (CO). The lithium dilution technique has seen increasing use and popularly among clinicians for good hemodynamic optimization. The technique is quick and simple, requiring an arterial line and central or peripheral venous access. These lines would usually already inserted in critical care patients. A small dose of lithium chloride is injected as an intravenous bolus, and cardiac output is derived from the dilution curve generated by a lithium-sensitive electrode attached to the arterial line.
Trend toward noninvasive cardiac stroke volume measurements. Minimally invasive cardiac output monitoring (MICOM) devices have gained vast clinical popularity, and are witnessing constant industry effort for technology innovations. The demand for noninvasive methods for the measurement of stroke volume (SV) and CO is a key driver for the expansion of the cardiac output monitoring devices market. Transthoracic echocardiography (TTE) also is emerging as a reliable technique for cardiac functional assessment, especially in the critical care setting. Transthoracic impedance and bioreactance analysis technologies also are expected to draw in sizable investment by manufacturers in the cardiac output monitoring devices market. The arterial waveform analysis technique has also acted as a mainstay in CO.
Transthoracic impedance (TI) can be measured by leads placed on the patient’s skin and represents the resistance of the thorax to current flow. Changes in tissue composition due to redistribution and movement of fluids induce fluctuations in the TI. Blood flow during the cardiac cycle generates small fluctuations synchronized to each heartbeat. Respiration (or assisted ventilation) also causes changes in the TI.
The resulting thoracic impedance graph, also known as an impedance cardiograph, indirectly reflects the volume changes of the heart and large vessels within the thorax, so it is closely related to the cardiovascular physiological activity and pathological changes. It is widely used to measure cardiac function and to monitor the hemodynamic changes.
Bioreactance is a newer, noninvasive method for cardiac output measurement that involves analysis of blood flow-dependent changes in phase shifts of electrical currents applied across the thorax. It can be used to assess hemodynamic variables.
Arterial waveform analysis allows for noninvasive calculation of derived parameters intrinsically created by a patients pulse pressure profile. These include estimates of left ventricular stroke volume, CO, vascular resistance, and during positive-pressure breathing, SV variation, and pulse pressure variation. In the past decade, arterial waveform analysis has gained a large interest in the overall assessment and management of the critically ill and those at a risk of hemodynamic deterioration.
Shift toward deep-learning in cardiac output monitoring. Minimally invasive CO monitoring relies on accurate quantification of stroke volume, among other parameters. The CO monitoring devices market has seen commercial use of analysis of the arterial waveform. However, more recently, healthcare providers have come to realize the numerous limitations the technique has. This has created the prospect of artificial intelligence (AI) and machine-learning (ML) techniques in SV, which has boosted the market for deep learning (DL) technologies.
Particularly, the market is expected to witness high adoption rates of DL-based SV estimations, especially for patients with hemodynamic instability. In coming years, more DL-based models will gather traction among physicians in getting a precise hemodynamic management in operational setting. For instance this may be useful in the intra-operative setting for CO monitoring in pregnant women.
However, catheter-based measuring will continue to see widespread use in healthcare settings.
Looking back to gain perspective on how far we have come is always a worthwhile effort. Indeed, cutting-edge programs will embrace the new and rejuvenated complexion of the cath lab and transition to the next clinically proven solution.











