CT Scanners
Role of CT scanners in diagnosing COVID-19
Radiologists have watched the COVID-19 pandemic unfold, wondering if and how imaging could be useful for diagnosis. Perhaps imaging could aid in screening and accelerating the speed of diagnosis.
Over the last decade, the diagnostic imaging industry has witnessed significant technological advancements in the field of computed tomography (CT), including the emergence of low-dose and automated CT scanners.
CT scan is a long-established imaging technique that has witnessed ample modifications and improvements over the past few decades. Significant evolution in this industry can be confirmed by the replacement of conventional systems by the 4th generation CT scanners.
Moreover, ongoing advancements in the field of semiconductor materials have enabled device miniaturization as well as the development of multi-slice CT scanners that offer 128-, 256-, 320-, or 500- slice CT images. These developments along with expansion in the application horizon of CT technology have resulted in their growing adoption among various end users worldwide.
Technological advancements have reduced the dose of radiation without hampering the quality of image. Such technological advancements coupled with the procedural benefits of CT scan over other imaging modalities like MRI and X-ray will stimulate its demand over forthcoming years.
Rising incidences of cardiovascular diseases globally will augment the CT scanners market growth in forthcoming years. Around 17.9 million people die annually due to cardiovascular diseases globally, according to WHO,. Disease burden and mortality rates have been significantly reduced due to accurate diagnosis of chronic conditions at early stages. As recently developed CT scanner allows the early and accurate diagnosis of several chronic diseases, its demand will grow in the near future. CT scanner is a cost intensive capital equipment and its high cost is expected to hamper affordability, particularly in developing and underdeveloped region that will restrain the CT scanner market growth.
A ROLE FOR CT IN COVID-19?
Can CT scans diagnose COVID-19? In addition to RT-PCR testing, some experts argue that CT scans can diagnose COVID-19. Others disagree.
As the COVID-19 pandemic continues to claim lives across the globe, early diagnosis of people with SARS-CoV-2 is essential. Once a person has received a diagnosis, limiting their physical contact with others is one way to slow the spread.
What is the best way of establishing a firm diagnosis for COVID-19?
For many, the use of reverse transcriptase polymerase chain reaction (RT-PCR) is the gold standard. This molecular biology technique detects genetic material that is specific for the SARS-CoV-2 virus. Yet, RT-PCR is not 100 percent accurate, and some experts have raised questions around false-positive and false-negative test results.
Could CT scans, which combine a series of X-ray images, serve as an alternative or an adjunct to RT-PCR diagnosis? There have been reports from Wuhan in China of healthcare professionals using CT scans to diagnose COVID-19, yet medical and public health bodies in the United States have not followed suit.
Arguing for the use of CT. The American College of Radiology (ACR) and the Centers for Disease Control and Prevention (CDC) based on false-positive rates, scanner contamination, and a lack of change in individual patient management have recommended against routine use of CT scans to diagnose COVID-19. However, in China, where experts quickly and effectively controlled the disease, professional medical organizations universally agree that CT plays a vital role in rapid identification, improved quarantining, and tailored public health measures.
Early on, in the COVID-19 outbreak, it became clear that RT-PCR testing is both slow and unreliable. One Chinese official estimated that swab test sensitivity was as low as 30 percent, a finding consistent with RT-PCR testing of fluid samples. More optimistic estimates from the ACR suggest a range of 42–71 percent for the RT-PCR test. In other words, the swab misses nearly a third of cases — at best.
According to a research article in Radiology, CT is far more sensitive, commonly detecting cases the swab misses. However, CT’s higher sensitivity (routinely estimated at well over 90%) and real-time results come at the expense of increased false positives.
But this downside is of far less concern to public health authorities than poor sensitivity. The World Health Organization’s strategic objective to stop human transmission of SARS-CoV-2 prioritizes the detection and isolation of potential spreaders above all else.
This focus on sensitivity, even at the cost of false positives, reflects the goals of pandemic medicine. Typically, doctors use diagnostic tests to benefit individuals, but the calculus of testing changes in epidemics. Experts in nations that endured SARS learned the hard way that rapid, sensitive testing is critical during an infectious outbreak not because of its benefit to individuals, but because it benefits everyone.
The focus of American experts on individual case management is well-intentioned and morally laudable. But the same logic quickly becomes dangerous during an epidemic. In transitioning to pandemic thinking, nations such as China saw that over-diagnosing COVID-19 was far better than under-diagnosing.
Moreover, the reason to diagnose COVID-19 is not patient management, it is pandemic management. The scans are not for the benefit of the person having the scan; they are for everyone else.
Detecting disease and quarantining is how we keep people without the infection safe. In other words, aggressively finding disease and isolating positives halts transmission, potentially saving not just one life, but many.
As for scanner contamination, China has no monopoly on cleaning techniques or technology. Their cleaning protocol allowed for the safe scanning of 200 patients each day on a single scanner with multiple clinics documenting zero transmissions to CT suite staff. This was one of many integral and necessary adaptations that yielded inarguable success. Their curve swiftly flattened, which saved countless lives.
Recommending against CT diagnosis for COVID-19, particularly during a shortage of swab tests in the U.S., was an unfortunate error that contributed to a period of unchecked, invisible spread of the virus. The U.S. now has the ignominious distinction of being the world leader in both cases and fatalities, with numbers still growing. In epidemics, a failure to control is virtually always a failure to detect.
There remains, however, a chance for redemption as we move into a phase of carefully repopulating public spaces while attempting to flatten the resultant mini-curves. Success will depend entirely on meticulous detection and quarantining of those infected.
Some radiology literature suggests a pivotal role for CT. Tao Ai and Zhenlu Yang alongwith their colleagues submitted their findings of a research on correlation of Chest CT and RT-PCR Testing in COVID-19 in China, a report of 1014 cases.
Results. Of 1014 patients, 59 percent (601/1014) had positive RT-PCR results, and 88 percent (888/1014) had positive chest CT scans. The sensitivity of chest CT in suggesting COVID-19 was 97 percent (95%CI, 95-98 percent, 580/601 patients) based on positive RT-PCR results. In patients with negative RT-PCR results, 75 percent (308/413) had positive chest CT findings; of 308, 48 percent were considered as highly likely cases, with 33 percent as probable cases. By analysis of serial RT-PCR assays and CT scans, the mean interval time between the initial negative to positive RT-PCR results was 5.1 ± 1.5 days; the initial positive to subsequent negative RT-PCR result was 6.9 ± 2.3 days). 60 percent to 93 percent of cases had initial positive CT consistent with COVID-19 prior (or parallel) to the initial positive RT-PCR results. 42 percent (24/57) cases showed improvement in follow-up chest CT scans before the RT-PCR results turning negative.
Conclusion. Chest CT has a high sensitivity for diagnosis of COVID-19 as compared with initial reverse-transcription polymerase chain reaction (RT-PCR) from swab samples in the epidemic area of China. Chest CT may be considered as a primary tool for the current COVID-19 detection in epidemic areas.
Having said this, no doubt RT-PCR to diagnose COVID-19 has some limitations: the test is not universally available, turnaround times can be lengthy, and reported sensitivities vary. Nevertheless, it is the accepted standard and only positive in patients who are infected with severe acute respiratory syndrome coronavirus. CT findings in patients with COVID-19, on the other hand, are seen with numerous pathogens and in many non-infectious aetiologies. Some experts believe CT does not add diagnostic value; positive results can only be believed if the pre-test probability of disease is high. Using CT diagnostically is not known to provide clinical benefit and could lead to false security if results are negative. If COVID-19 is suspected, patients should be isolated pending confirmation with (multiple) RT-PCR tests, or until quarantine has lapsed. The results of a CT scan do not change this.
Framing CT as pivotal for COVID-19 diagnosis is a distraction during a pandemic, and possibly dangerous. Safely using CT to study COVID-19 patients is logistically challenging and can overwhelm available resources. Some experts urge caution and encourage using published guidelines regarding use of CT imaging.
Indian market
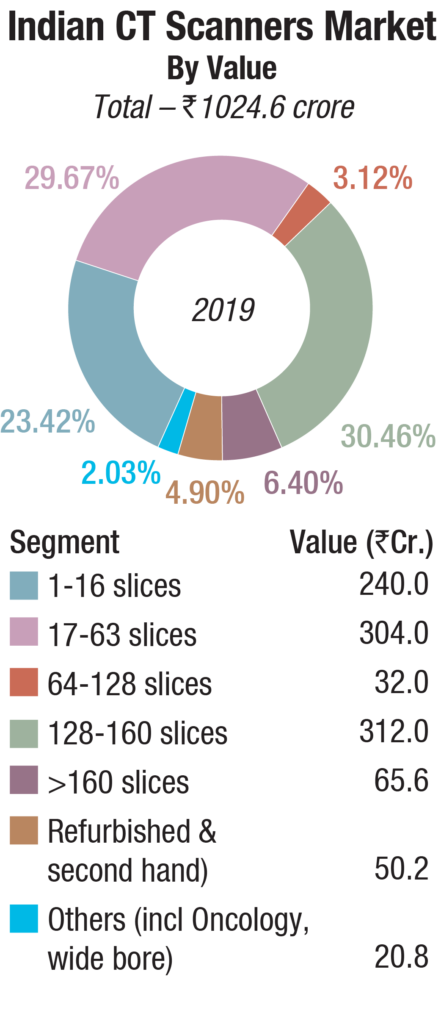
The Indian market for CT scanners in 2019 is estimated at Rs 1024.6 crore, with 725 units. This is a 17.16-percent decline by value and an 8.8-percent decline by volume in 2019, over 2018.
The major gainer in 2019 was 17–63 slice scanners, which saw a 7.5-percent increase in the market share. The 64–128 slice CT scanners saw a 2.8-percent increase, the 128–160 slice scanners a 6.7-percent, and the >160 slice scanners a 2.8-percent increase in market share in 2019, over 2018. They seem to have taken share from the 1–16 slice category, which saw a 14.25-percent drop and the oncology and wide-bore CT scanners.
Indian CT Scanners Market |
||||
|---|---|---|---|---|
Leading players* – 2019 |
||||
| Tier I | Tier II | Tier III | Tier IV | Others |
| GE | Siemens | Philips | Toshiba, Hitachi, Allengers and a small presence of Chinese brands. | Carestream Health, Samsung, Medirays, Schiller, Shimadzu, and Trivitron |
| *Vendors are placed in different tiers on the basis of their sales contribution to the overall revenues of the Indian CT scanners market. | ||||
| ADI Media Research | ||||
GE is a clear leader in the segment. Siemens comes next, followed by Philips. Other brands, which have presence, are Erbis (Toshiba) and Hitachi, both brands finding more popularity with government procurement, and Allengers and a minor presence of some Chinese brands. 2020 saw aggressive marketing from Medirays Corporation for its Instium scanners and United Imaging, a brand headquartered in Shanghai, but with strong presence in USA.
 Global market
Global market
The size of the global CT scanners market was worth USD 6.6 billion in 2019 and it is estimated to reach USD 8.2 billion by the end of 2024, at a CAGR of 4.54 percent during 2019–2024, estimates Market Data Forecast. With the advent of high-speed and multi-slice CT scanners, healthcare providers have changed their approach to imaging, diagnosis and treatment of patients as new ways for clinical applications in such areas as trauma, vascular, pediatric, and cardiac imaging are possible due to the higher speeds at which scanning can be done. CAD software has been pivotal in bringing new applications to CT, for example, making cancer detection possible with CT.
Rapidly growing demand for bedside imaging, home healthcare, and growing use of CT scan to assess the accuracy of post-interventional medical procedures, medical implants, and anatomical confirmation are some of the main factors driving industry growth. Increasing prevalence of diseases like cancer, orthopedic, cardiovascular, and dental disorders will also enhance the growth of the CT scan market. Also, a never-ending increase in the number of medical implants surgeries owing to unhealthy lifestyles as well as a growing base of geriatric population is likely to increase demand.
Other drivers of growth include the growing demands from governments for premium healthcare delivery. Significant advances in imaging technologies promise to improve wellness through quicker and more precise detection of medical conditions. A rising fiscal deficit is expected to hinder the growth of the CT scanners market in developed nations. Also, the CT imaging radiation dose continues to be an area of concern. A lot of patients and medical associations have raised this issue and raised their voices against the possible side-effects of CT scanning. The industry continues to try to reduce exposure while ensuring image quality.
The multi-slice feature has evolved CT from simply a diagnostic tool into an interventional modality. Though most of the CT scanners are still used as general systems, some are being modified for specific purposes like bone densitometry or cardiovascular studies. The innovation cycle of CT has become indeed very short with new and cutting-edge technology is getting introduced in the CT scanner market with each being more efficient and faster. There is an increasing demand for high slice CT. The high slice CT scan is expected to improve the clinical utility considerably, as the introduction of 256 slice scanner, which has a detector width of 10 to 12 cm would help in scanning organs, including the brain, heart, entire joints, and lungs and liver, within a single rotation. It is also expected to have the feature to scan the heart with a single heartbeat.
Based on low-slice type, the single slice segment is witnessed in holding the highest shares of the market. The rise in the number of patients’ suffering from chronic and infectious diseases is prompting the demand of the market. Increasing awareness over the utilization of advanced devices is leveling up the growth of the market.
On the basis of high-slice type, 40-slice category, in high slice type is leading with dominant shares of the market with the growing prevalence for the medical implants. Adoption of sedentary lifestyles and changes in food habits is likely to bolster the demand of the market.
Hospitals and clinics end-user have dominant shares of the market, on the basis of end-users. Increasing support from the government through investments in the constructional activities of the healthcare centers is lavishing the demand of the market. Also, the growing demand for quality diagnostic procedures is boosting up the growth of the CT scan market.
North America is witnessed in holding the highest shares of the global CT scanners market with the quick adoption of advanced technology and the introduction of various devices in favor of the patient’s safety. With modern techniques, the devices are allowing the patient to have lower exposure to higher radiations which promotes fewer side effects is enhancing the growth of the market in this region. Also, raising capita income in developed and developing countries is leveraging the growth of the market.
The Asia Pacific is following North America in dominating the largest shares of the market by owing to the increasing aging population. Besides, increasing risks from colon cancer are escalating the demand for the CT scan market. Europe is accounted for in having an enormous growth rate and is also to have better growth opportunities in the coming years. Increasing expenditure on healthcare and to have effective treatment procedure at any cost are boosting up the growth rate of the market in this region.
Recent advancements
Many will undergo a CT scan at some point in their lifetime — being slid in and out of a tunnel as a large machine rotates around. CT is a widely used method of obtaining cross-sectional images of objects. A research team led by Tohoku University Professor, Wataru Yashiro has developed a new method using intense synchrotron radiation that produces higher quality images within milliseconds.
High-speed, high-resolution X-ray CT is currently possible using intense synchrotron radiation. However, this requires samples to be rotated at high speed to obtain images from many directions. This would make CT scans more akin to a rollercoaster ride!
Extreme rotation also makes controlling the temperature or atmosphere of the sample impossible.
Nevertheless, the research team solved this conundrum by creating an optical system that splits single synchrotron X-ray beams into many. These beams then shine onto the sample from different directions at the same time; thus, negating the need to rotate the sample.
This multi-beam method is no easy task since the direction of X-rays cannot be easily changed. Unlike visible light, X-rays interact with matters weakly, making it difficult to utilize mirrors and prisms to change the path of the beams.
To overcome this, the research team used micro-fabrication techniques to create uniquely shaped crystals. These crystals were then bent in the shape of a hyperbola. By combining three rows of crystals, the multi-beam optics were able to cover an angle of ±70°.
Carrying out their experiments at the SPring-8 synchrotron radiation facility, the research team took advantage of a cutting-edge compressed-sensing algorithm that needs only a few dozen projection images for image reconstruction.
The invention makes 3-D observations of living beings and liquid samples within milliseconds possible. It is possible application is widespread, from fundamental material science to life sciences to industry.
Future of CT
In recent years, much work has been done to improve upon CT, but there are more innovations on the way that will impact providers and augment patient care.
CT was considered a mature technology through the mid to late 1980s. For a few years, CT development seemed to slow again until 1998 when multidetector-row CT emerged, allowing acquisition of isotropic imaging volumes that expanded image interpretation beyond primary transverse reconstructions to volumetric visualization and analysis. Novel applications emerged into mainstream practice expanding CT into new clinical roles for lung cancer screening, coronary artery disease diagnosis, and characterization of cerebral ischemia.
After the row races slowed down and radiation exposure rose as a concern, iterative reconstruction and low kV imaging emerged to reduce radiation dose by as much as an order of magnitude. The demand for higher temporal resolution to freeze cardiac motion was met with faster gantry rotations, dual-source geometries, and post-processing algorithms. Finally, dual-energy CT acquisition introduced us to simulated monoenergetic reconstructions and material decomposition, albeit with caveats for those hoping to reliably create virtual unenhanced images and remove arterial calcification from arterial walls.
So, what new CT platform advancements will appear to initiate the next wave of clinical innovations and when might we expect them?
In the near term, major source redesign is unlikely, but we can expect continued increases in power output from smaller X-ray tubes. These advances should bring further increases in gantry rotation speed, improving temporal resolution for cardiovascular applications. While highly novel field and photo emission sources have been developed and entice us with the prospect of radical redesigns of the entire CT system, their appearance in the clinic is likely to be beyond a five year horizon.
In contrast to the source and gantry systems, industry is at the cusp of a major advancement in detector technology. Early experimentation visualizing gold nanoparticles for blood pool imaging as well as passively and actively targeted tumor imaging have been enabled using multispectral techniques.
As exciting as these advancements have been, photon-counting detectors (PCDs) are poised to greatly improve and expand these capabilities. Currently prevalent in SPECT, PET, and small-bore CT systems, PCDs must be designed differently to accommodate the higher photon flux of CT systems, but progress is being made.
Energy integrating detectors intrinsic to current clinical CT systems rely on the conversion of visible light to electrical signals through a chain that flows from scintillator to photodiode with the resultant output being proportional to the total energy of the detected photons.
Thus, higher energy photons contribute more to the output signal than low energy photons. In contrast, PCDs directly convert the energy of X-ray photons to electric energy. Because a scintillator is no longer needed, detector elements can be smaller and packed tighter providing a basis for scans with higher spatial resolution than currently available.
Moreover, PCDs count incident photons discretely, providing a means of measuring and then binning each photon detection into one of 2–8 bins based upon its energy with the number of bins being determined by the PCD’s design.
The potential clinical payoffs of PCDs are many. A reduction in electronic noise will provide high-quality images using lower radiation exposure and in larger patients. Higher spatial resolution could improve a variety of applications particularly in assessing pulmonary, osseous and cardiovascular structures.
This includes metallic implants such as stents and stent-grafts as well as characterization and measurement of atherosclerotic plaque and its influence on luminal dimensions.
Finally, multi-spectral applications will be acquired with complete spatial and temporal registration using a single X-ray source, tube potential and detector layer, eliminating many current limitations.
User-defined energy thresholding will enhance flexibility, allow greater selection and post-scan filtering of iodine and calcium. The application will also optimize discrimination of novel contrast agents, allowing new applications based upon the simultaneous discrimination of multiple contrast agents.
One intriguing advance that offers a fundamentally different contrast mechanism from current attenuation-based clinical systems bears mention. Phase-contrast CT images the deflection of photons that undergo Compton scattering and produces novel tissue contrast that accentuates tissue interfaces both at macroscopic and microscopic scales. It is also capable of quantifying electron density as a basis for material classification.
Although its clinical adoption in a whole-body system is likely to be more than 5 years off, one may see an earlier translation to small systems dedicated to breast or extremity imaging.
For most of CT’s evolution, detectors, tubes and gantries have grabbed the headlines, while software served as supporting cast to the hardware. However, data collection subsystems and associated software refinements have played a largely unsung role in advancing CT technology.
However, these improvements are expected to pale with the growing incorporation of machine learning (ML) techniques for the control and analysis of CT data.
In sum, the industry stands at the cusp of a number of transformative CT innovations that experts can anticipate will bring fundamental changes to the technical capabilities and clinical applications of this diagnostic workhorse.
Second Opinion
 Dr Vijay Kumar Agrawal
Dr Vijay Kumar Agrawal
Director – Critical Care Medicine and Academic Programs,
Metro Heart Institute
CT vs. RT-PCR
The virus that causes COVID-19 is designated SARS-CoV-2, and the understanding of COVID-19 is still evolving. Although the diagnosis of COVID-19 is made by detection of SARS-CoV-2 RNA by RT-PCR, it has rigorous laboratory specification and requires a long time before results are available. Additionally, some suspected COVID-19 patients may have initial false-negative results on nucleic acid testing, which is harmful for the control of infectious disease. Serologic tests detect antibodies to SARS-CoV-2 in the blood, but their major role is in large-scale serologic screening.
Chest CT scan may be more sensitive than chest radiograph, and some chest CT findings may be characteristic of COVID-19. CT chest features have been categorized as typical, indeterminate, or atypical for COVID-19. Chest CT in patients with COVID-19 most commonly demonstrates ground-glass opacification with or without consolidative abnormalities, consistent with viral pneumonia. Ground glass (GGO) pattern is the most common finding in COVID-19 infections. They are usually multifocal, bilateral, and peripheral, but in the early phase of the disease the GGO may present as a unifocal lesion, most commonly located in the inferior lobe of the right lung. Sometimes, there are thickened interlobular and intralobular lines in combination with a ground glass pattern.
This is called crazy paving. It is believed that this pattern is seen in a somewhat later stage. Vascular dilatation with a typical finding of widening of the vessels in the area of ground glass may be seen. Another common finding in the areas of ground glass is traction bronchiectasis.
In some cases, there is architectural distortion with the formation of subpleural bands. Pleural effusion, pericardial effusion, lymphadenopathy, cavitation, CT halo sign, and pneumothorax are some of the uncommon but possible findings seen with disease progression. The severity of lung involvement on the CT correlates with the severity of the disease. The severity on CT can be estimated by visual assessment or by scoring the percentages of each of the five lobes that are involved.
In a study of 1014 patients in Wuhan, who underwent both RT-PCR testing and chest CT for evaluation of COVID-19, a positive chest CT for COVID-19 had a sensitivity of 97 percent, using the PCR tests as a reference; however, specificity was only 25 percent. The low specificity may be related to other aetiologies causing similar CT findings, especially other viral pneumonias. In another study comparing chest CTs from 219 patients with COVID-19 in China and 205 patients with other causes of viral pneumonia in the United States, a group of radiologists were able to distinguish COVID-19 with high specificity but moderate sensitivity. Chest CT abnormalities have also been identified in patients prior to the development of symptoms, and even prior to the detection of viral RNA from upper respiratory specimens.
In conclusion, although chest CT may be more sensitive than chest radiograph, and some chest CT findings may be characteristic of COVID-19, no finding can completely rule in or rule out the possibility of COVID-19. There is much overlap of the CT-pattern of COVID-19 with other viral pneumonias. CT had a low rate of missed diagnosis of COVID-19, and thus may be useful as a standard method for the diagnosis of COVID-19 based on CT features and rules of transformation. Also, rapid diagnosis can lead to early control of potential transmission.
 Dr Abhijit Patil
Dr Abhijit Patil
Prof. & HOD Dept. of Radiodiagnosis,
SMCW & SUHRC
Need for AI parenting
Trends as it may seem may not always be advancement, as COVID-19 has taught us how important it is to stick to basics as general hygiene, immunity, cleanliness, etc. Nevertheless, it is imperative that we make regular advancements in technology, hardware, and software, and help the people in the field stay updated with these and implement them in practice. Researchers have spent a lot of time and money in many aspects of this like speed and quality of image acquisition, patient and operator safety, post-processing, and data storage and retrieval. It would wow anyone a decade or two ago if it was said all this could occur at ‘the click of a button’. But in this age of smartphones, in which technology is evolving every day, it is expected that the button be clicked only once and not at every stage. With this perspective hyper-automation in radiology [including artificial intelligence (AI) and machine learning (ML)], 3D image printing, and virtual reality (VR) have replaced discussions on image acquisition, post processing, etc., as seen in RSNA 2019.
Implementation of AI and ML requires advancementin robotics software as well as patient data-handling. AI was already in practice knowingly or unknowingly at the end of the last century, when we had started using search engines on the internet. The leading vendors in manufacturing of imaging equipment are also integrating their hardware and picture archiving and communication system (PACS) with their own or third-party AI platforms. This extends from selection of protocols to aid workflow, image post-processing as automatic reconstruction, display of primary AI results segregating normal from abnormal, sending all the information to PACS, thus theoretically leaving the radiologist only the task to finalize the reports. However, as we know with advancement in technology, implementation of AI and ML has brought forward newer challenges of cybersecurity, malware, data storage and retrieval for medicolegal purposes, intellectual property rights (IPR), etc. There is still confusion weather AI platforms need validation from medical research or information technology, or maybe from both departments for their authenticity and medicolegal validity. This calls for experts to draft rules and regulations for standardization not only acceptable in our country but also internationally, as has been done for other aspects of medicine. Thus, the need for artificial intelligence parenting.












